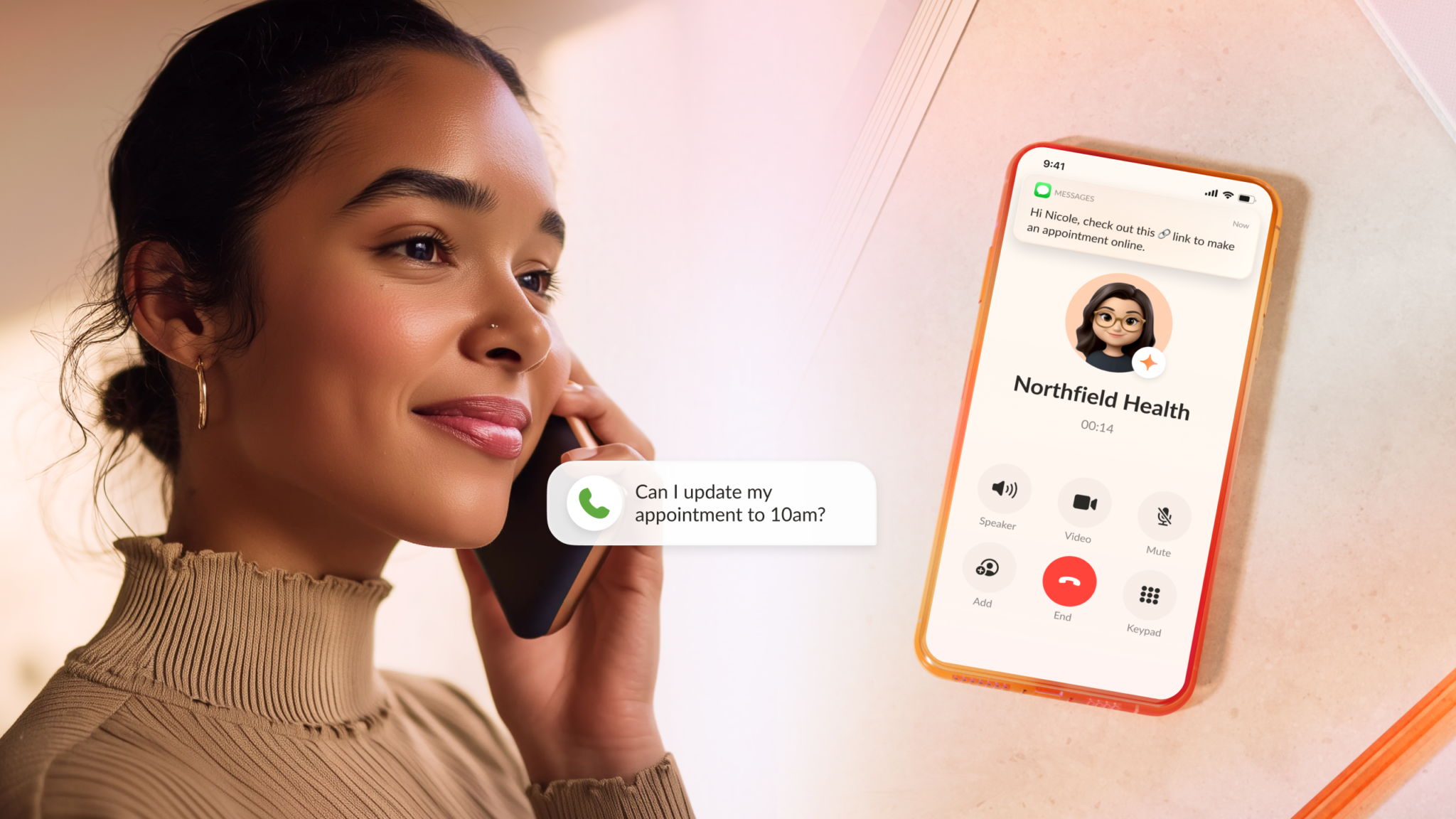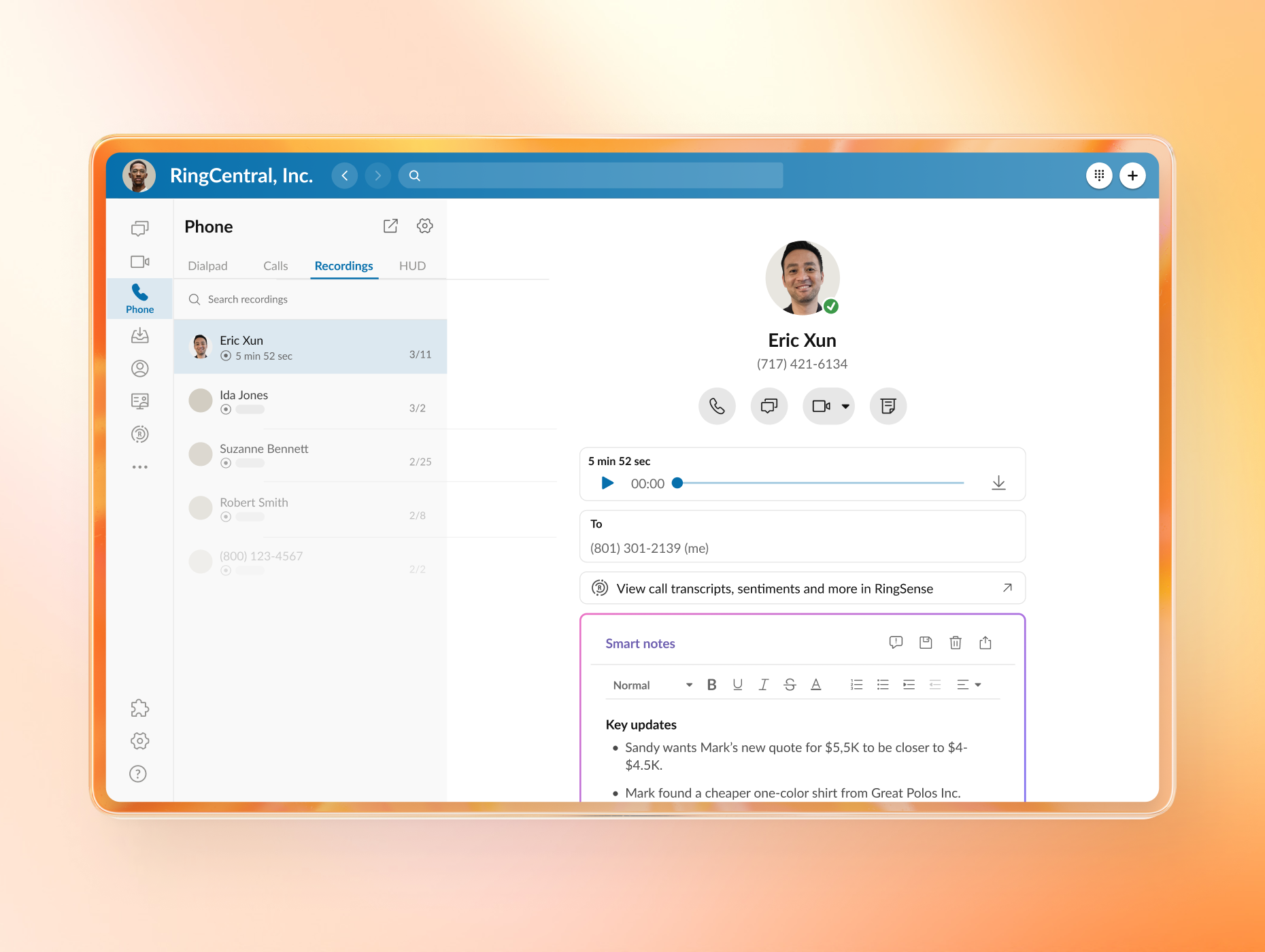
Today, we’re launching RingCentral AIR Pro (AI Representative), a voice-first, omnichannel conversational AI agent and orchestration studio designed to automate ...
4 min read
Latest stories

A trusted leader in global AI communications
Discover how RingCentral's AI-powered communications can transform your business today.
Learn more Content Hub
Access a range of ebooks, whitepapers, infographics, and more to stay informed and ahead in the world of AI-powered communications.
Collections
Discover curated collections of articles, case studies, and resources for easy access to related content and insights
Industry Spotlight
How to elevate customer experience in banking with AI and automation
Learn how voice-first AI, unified communications, and intelligent automation help you deliver seamless, secure customer experiences across every channel. Modern customers expect instant ...
9 min read
Healthcare call center software for faster patient access in 2026
What to look for to reduce wait times, automate routine tasks, and protect patient data. Running patient access, IT, or contact center operations means navigating competing pressures all day. ...
8 min read
How a retail contact center transforms customer experience in 2026
Learn how to unify your channels, deploy voice-first AI, and turn every customer interaction into a revenue opportunity. Modern customers jump from TikTok and mobile apps to store associates and ...
11 min read
Transforming law firm communications with digital fax solutions
Law firms have long relied on traditional communication methods like fax machines and Plain Old Telephone Service (POTS) lines to handle sensitive client information. However, as technology ...
3 min read
10 simple student voice strategies
Highlights Students are the foundation of your school, but often, their voices are underrepresented. Supporting student voice leads to more student engagement, and ultimately to better school ...
4 min read
This rural Virginia county government went from spotty phone service to world-class cloud communications
Highlights:
Enabling telework: Surry County’s government employees can now reliably call, message, text, video chat, and fax from anywhere, using any device.
Improving service: With ...
4 min read
Browse all
Filters
- AI & Innovation
- Business & leadership
- Communication & collaboration
- Company news & culture
- Customer & employee experience
- Customer stories
- Education
- Events
- Financial services
- Global Strategic Partnerships
- Government
- GSP
- Guiding principles for the modern enterprise
- Healthcare
- IT
- IT leadership
- Law
- Marketing
- Mastering sales and marketing
- Mobility
- Open platform
- Professional services
- Real estate
- Retail
- Sales
- Security
- Service & support
- Small Business Growth Tactics
- Startups
- Telehealth

Curious about about our solutions?
Discover how RingCentral's AI-powered communications can transform your business today.
Learn more