Learn how to build patient engagement that reduces no-shows, streamlines operations, and improves margins.
Your patients expect Amazon-level convenience, and your board expects better margins. But your staff can’t deliver on either without the right infrastructure.
Fragmented communication channels and siloed data frustrate your patients, burn out your teams, cost you revenue, and tank your Hospital Consumer Assessment of Healthcare Providers and Systems (HCAHPS) scores. Implementing patient engagement as an enterprise capability instead of patching together point solutions unlocks a direct line from operational efficiency to clinical excellence.
This guide explains how to design, implement, and scale effective patient engagement strategies built on unified communication, real-time data, and AI—the foundation you need for 2026 and beyond.
Key takeaways
- Unifying communications, data, and AI reduces no-shows, improves HCAHPS scores, and unlocks operational capacity
- Developing patient engagement as a strategic capability delivers measurable ROI and sustainable workforce efficiency
- Choosing platforms with embedded security and interoperability allows you to scale proven workflows without rebuilding your tech stack
- Integrating real-time data and AI into digital portals transforms passive tools into active orchestration engines for care coordination
What are patient engagement strategies?
Patient engagement strategies are systematic frameworks that align technology, data, and communication to involve patients in care delivery. At the enterprise level, they go beyond reminder texts and portals by transforming engagement into a core capability that drives operational and financial performance.
Patient engagement strategies define how healthcare organizations:
- Reach patients across phone, SMS, email, portal, app, and video before and after every caregiver encounter
- Use data to understand each patient’s needs and communication preferences
- Orchestrate workflows across clinical, operational, and contact center teams to deliver a single, coherent care management journey
- Embed security, privacy, and compliance into every interaction, including AI-driven outreach and in-person clinical consults
Patient-centered engagement strategies deliver measurable outcomes. Proactive outreach reduces no-shows and readmissions, while streamlined scheduling unlocks capacity and improves HCAHPS scores. Clinicians and staff benefit, too, from fewer manual calls, follow-ups, and duplicate tasks.
For leaders, the systems that enable these efforts are an investment in ROI. Contact center platforms, digital front-door tools, and AI reduce leakage, increase throughput, improve quality metrics, and optimize workforce efficiency. A clear enterprise strategy helps you prioritize capabilities, measure impact, and avoid adding another siloed tool.
7 patient engagement strategies that drive measurable results
Enterprise-scale patient engagement requires a foundation that connects communications, data, and workflows across clinics, hospitals, virtual care, and home health.
These seven strategies leverage that foundation to deliver the operational efficiency, clinical outcomes, and patient satisfaction your organization needs:
1. Unify communications across every channel and touchpoint
Cloud-based voice, messaging, and video connect contact centers, front desks, care teams, and the back office on a single platform to eliminate scattered phone systems and point solutions.
This provides consistent patient communication whether they call, text, or use your portal, and lets staff work from one high-quality interface.
2. Build a flexible data and integration layer
Application programming interfaces (APIs), event streaming, and Health Level Seven (HL7) and Fast Healthcare Interoperability Resources (FHIR) integration tie your customer relationship management (CRM) platform, contact center, and digital health tools into one ecosystem.
Real-time data exchange means patients see accurate appointment availability, staff access complete context during every interaction, and systems stay synchronized without manual updates.
3. Deploy AI and analytics that drive action
Models and automation trigger outreach, influence routing, and guide staff dynamically based on patient context. This shifts operations from passive dashboards to active orchestration: identifying high-risk patients before they miss appointments, surfacing sentiment trends from call transcripts, and automating routine tasks so teams can focus on complex health conditions.
4. Design configurable workflows that adapt to your operations
Low-code or no-code capabilities let operations, access, and customer experience (CX) teams adjust engagement journeys without long development cycles. This agility enables testing new approaches, refining based on results, and deploying proven workflows across locations without waiting for IT resources.
5. Embed enterprise-grade security and governance
Consistent identity, access, consent, and auditing across all channels keep you aligned with Health Insurance Portability and Accountability Act (HIPAA), organizational policies, and emerging AI regulations. Clear governance standards reduce risk, accelerate rollout, and enable local innovation within safe boundaries.
6. Make digital platforms and portals your engagement foundation
Your digital health platforms and patient portals serve as the front door to your engagement strategy. When these tools lack tight integration or intuitive design, patients default to high-cost phone channels or disengage entirely.
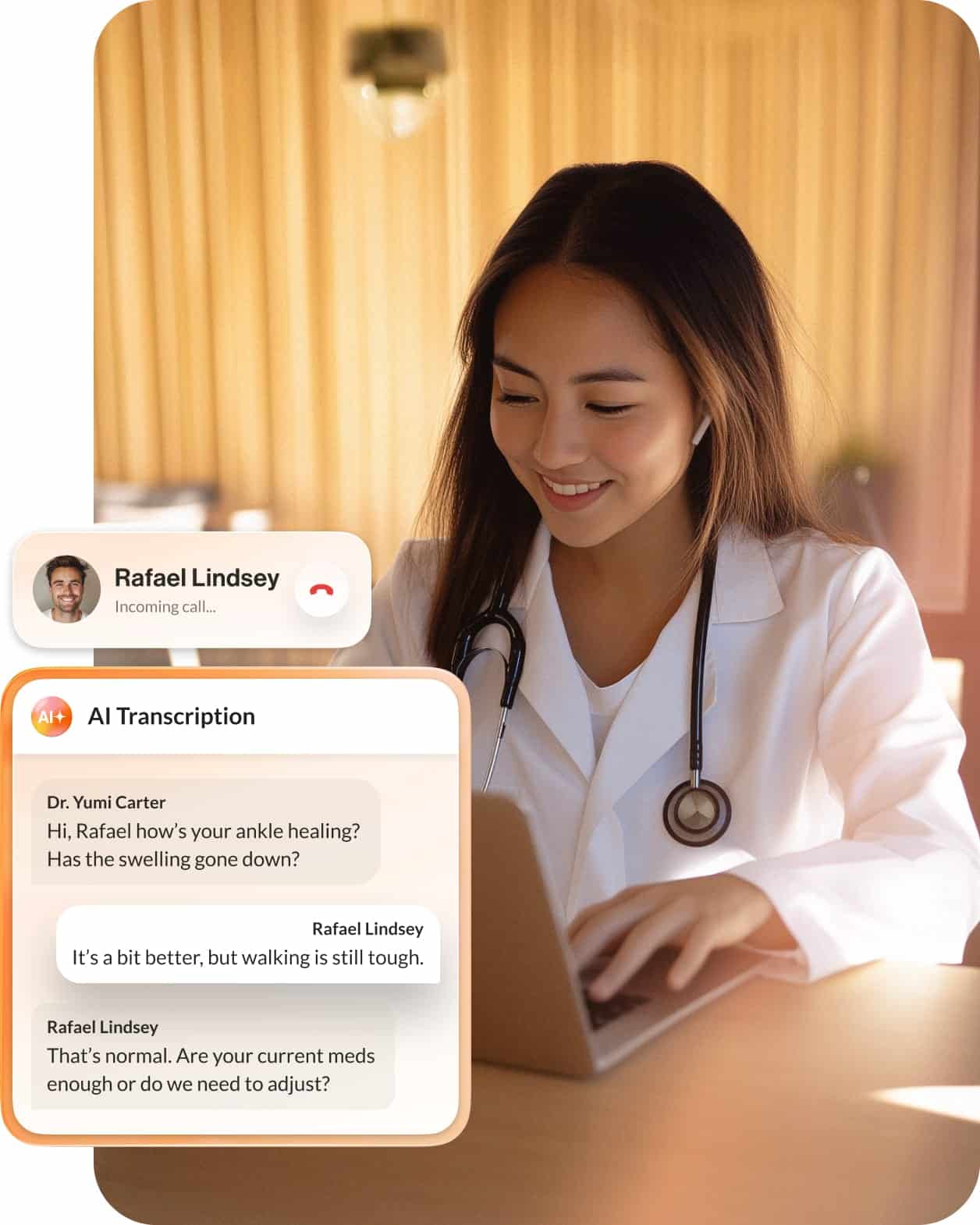
To make digital platforms central to your patient engagement strategy, focus on three areas:
- Deep integration with core systems: Connect portal and digital front-door tools bidirectionally with electronic health record (EHR), scheduling, billing, and communication platforms. This delivers real-time appointment availability, accurate visit preparation instructions, up-to-date test results, and secure messaging that care teams see in their native workflows.
- Experience design that reduces friction: Deliver consumer-grade simplicity through intuitive navigation, single sign-on, mobile optimization, accessibility features, and clear language. Maintain consistent communication templates and content governance so patients see the same information across your portal, website, and contact center.
- Voice-enabled and AI-supported access: Employ voice-enabled channels that let patients schedule, confirm, or change appointments, get directions, or access basic triage via a simple call. Use AI agents to extend this experience into chat and SMS, providing 24/7 self-service while escalating complex issues to live staff.
Support the entire conversation lifecycle: before visits (discovery, scheduling, intake), during encounters (shared decision-making, language services), and afterward (follow-up, results, refills, payments) without forcing patients to repeat their story. Design your digital platforms and voice channels as one unified system to deliver this continuity at scale.
7. Personalize experiences with integrated data analytics
Personalization in healthcare means tailoring timing, channel, content, and support based on clinical, behavioral, and operational data to empower patients to better manage their own health.
Build this capability with a data and analytics approach that drives action:
- Real-time data processing: Capture events as they happen and surface that information across channels instantly.
- Predictive analytics and segmentation: Identify patients at higher risk of no-shows, readmissions, or disengagement using historical data, then prioritize outreach for those groups.
- Conversation intelligence: Analyze call recordings and transcripts to surface common issues, sentiment trends, and friction points.
- Action-oriented automation: Trigger workflows based on analytics—send pre-op instructions via SMS, route high-risk patients to specialized nurse lines, or offer self-service to low-acuity callers.
Connect analytics to your communication and workflow engines to shift from passive reporting to active orchestration. Patients receive relevant outreach, staff focus on the right tasks, and leadership gains a clear line of sight from data to better health outcomes.
How to implement patient engagement strategies across enterprise healthcare systems
At enterprise scale, improving patient engagement requires coordination across service lines, regions, and business units. Without clear ownership and a structured rollout, even well-designed strategies fail.
Turn strategy into repeatable practice with this implementation framework:
Step 1: Define vision and outcomes
Align executives on success metrics. Target improved access, reduced call volume, higher portal adoption, or better HCAHPS scores, then translate goals into measurable KPIs and a three-year roadmap.
Step 2: Map patient journeys
Choose high-impact journeys like new patient onboarding or surgical interventions. Map every touchpoint across channels, then identify pain points, handoff failures, and redundant communication.
Step 3: Consolidate your platform stack
Inventory existing communication tools, portals, CRMs, and engagement solutions. Consolidate around a unified communications and contact center platform that integrates with your EHR and digital front door instead of adding standalone tools.
Step 4: Build cross-functional teams and governance
Establish cross-functional governance with shared decision rights across clinical, operational, and technology teams. To do this, create a patient engagement council with executive sponsors (CIO/CTO and CMO or VP of Patient Experience), operational leaders from access and revenue cycle, clinical stakeholders, technology and data teams, and compliance experts.
Define governance standards for channel usage, message templates, consent management, AI policies, and escalation rules to reduce risk, accelerate rollout, and ensure a unified brand voice.
Step 5: Ensure interoperability and seamless data exchange
Prioritize technical integration to prevent initiatives from stalling. If your engagement tools can’t talk to your EHR, scheduling, billing, and communication systems, patients receive conflicting information and staff resort to manual workarounds.
Focus on four technical priorities:
- Standards-based integration: HL7 FHIR, RESTful APIs, and event-based messaging let systems share patient data, appointments, and task updates securely.
- Identity and matching: Master patient index practices and identity management integration ensure you’re engaging the right person regarding the right health information.
- Open, extensible platforms: Cloud platforms with published APIs and healthcare-ready integrations let you embed calling, messaging, and AI directly into EHR workflows.
- Reliability and security: Enterprise-grade service-level agreements (SLAs), encryption, role-based access controls, and geo-redundant infrastructure keep channels available and compliant.
When your communication layer is interoperable by design, you can add new capabilities without rebuilding your stack.
Step 6: Pilot, then scale
Launch a focused pilot in one region with defined success metrics. Refine workflows, governance, and training based on results before expanding to additional sites.
Step 7: Build continuous improvement
Treat engagement as a living program by scheduling regular reviews to assess performance, test new approaches, and adjust workflows.
Centralizing cloud phone, collaboration tools, and contact center capabilities on a single platform ensures data flows directly into clinical and operational workflows. This integrated architecture allows you to deliver consistent experiences across patient populations and locations while simplifying rollout, standardization, and governance.
How to measure the impact of patient engagement initiatives on operational and clinical outcomes
Without clear metrics, patient engagement programs tend to become secondary priorities. To demonstrate how your strategies influence both patient outcomes and operational health, consider these four domains:
- Patient experience and access: Measure call answer rates, speed to answer, first-contact resolution, digital channel adoption, and self-service completion. Track satisfaction scores at key touchpoints like scheduling and post-discharge follow-up.
- Clinical quality and safety: Monitor readmission rates, time-to-follow-up after discharge, screening completion, patient care plan adherence, and care gap closure driven by outreach.
- Operational efficiency and financial impact: Evaluate appointment utilization, no-show rates, average handle time, call deflection to self-service, communication-related overtime, and revenue cycle performance.
- Workforce experience: Track turnover, schedule adherence, quality scores, and task burden. Effective engagement workflows reduce repetitive work and boost staff satisfaction.
Modern communication platforms collect and analyze this data automatically by categorizing calls by intent, flagging friction points like confusing interactive voice response (IVR) menus, and tracking sentiment trends. These automated insights fuel a closed-loop process: establish baselines, pilot new workflows, compare outcomes, refine based on transcripts and surveys, and roll out proven patterns across locations.
Future trends for patient engagement in healthcare
AI advances, consumer expectations, and regulatory shifts are reshaping patient engagement. When it comes to building engagement that scales safely and adapts quickly, four trends define the next phase:
Voice-first and agentic AI experiences
Patients now expect natural language interactions for routine tasks, and results are promising. A recent chatbot study found that one vendor’s conversational AI achieved an engagement rate of over 90% among enrolled patients due to ease of use.
AI embedded in clinics, hospitals, and homes
AI synthesizes data across systems to support triage, care navigation, and health management coordination. Clinics like Helix Urgent Care in Florida have already seen improvement after folding AI into their processes and systems—by using RingCentral’s AI Receptionist (AIR), Helix Urgent Care started saving 13 front desk hours a week, with 64% of calls answered by AIR.
Tighter governance and compliance requirements
Regulators are scrutinizing AI, data sharing, and information blocking. A Deloitte survey found that 80% of health system executives expect generative AI will have a moderate-to-significant impact on their organizations and agree that regulatory oversight of gen AI is necessary. Establishing clear policies on patient data use, human oversight of AI decisions, and consent management across every channel is essential.
Platform consolidation over point solutions
Creating effortless patient experiences is now a requirement for retention. Accenture’s loyalty survey found that patients who find their provider easy to work with are 84% more likely to stay than those who don’t.
To support engagement, health systems are replacing fragmented tools with open, interoperable platforms. Allowing connected systems to share data like health records and treatment options improves patient access and provides a more consistent experience.
The biggest decision is identifying the partners that can evolve with you. Choose vendors that deliver unified communications, digital and voice contact centers, and AI-driven engagement in ways that meet healthcare’s security, reliability, and compliance standards.
Build patient engagement that delivers results
Enterprise patient engagement comes down to three imperatives: unify your communication channels, connect data in real time, and embed AI where it drives measurable impact. Execute on these fundamentals to reduce no-shows, improve HCAHPS scores, unlock capacity, and give your teams the tools they need to focus on high-value work, like RingCentral’s suite of solutions:
- RingEX delivers secure, cloud-based voice, messaging, and video for clinical and operational teams.
- RingCX unifies patient-facing contact centers with voice, digital channels, and AI tools to create consistent experiences across access, billing, and care coordination.
- AI Receptionist (AIR) answers inbound calls and uses context to effectively route them to the right team or department, as well as performing automatic, routine calls like appointment scheduling and follow-ups.
- AI Virtual Assistant (AVA) provides clear notes, summaries, and insights to internal teams for greater task management and productivity.
- AI Conversation Expert (ACE) performs interaction analyses and curates coaching insights for each conversation.
Explore how RingCentral’s healthcare communications platform simplifies architecture while meeting healthcare’s security, reliability, and compliance standards. The foundation you build today determines whether you deliver coordinated, intelligent engagement that improves outcomes, strengthens loyalty, and makes work sustainable for your teams.
Originally published Mar 17, 2026