A practice that’s ever-growing in popularity, telemedicine is an innovative way to connect to patients. You may have heard the term telemedicine or telehealth before. You may be in a position where you either want to know more about it, or you are ready to delve into this interesting and modern world of providing medical care.
Telehealth is the use of technology in general to promote health. For example, perhaps the government may decide to do a text campaign promoting healthy eating. Whilst telemedicine is a specific offshoot from telehealth. Telemedicine is when health care providers use technology, like video calls, to give medical care to patients who can’t make it into a hospital or doctor’s office for one reason or another.

Source: Business Wire
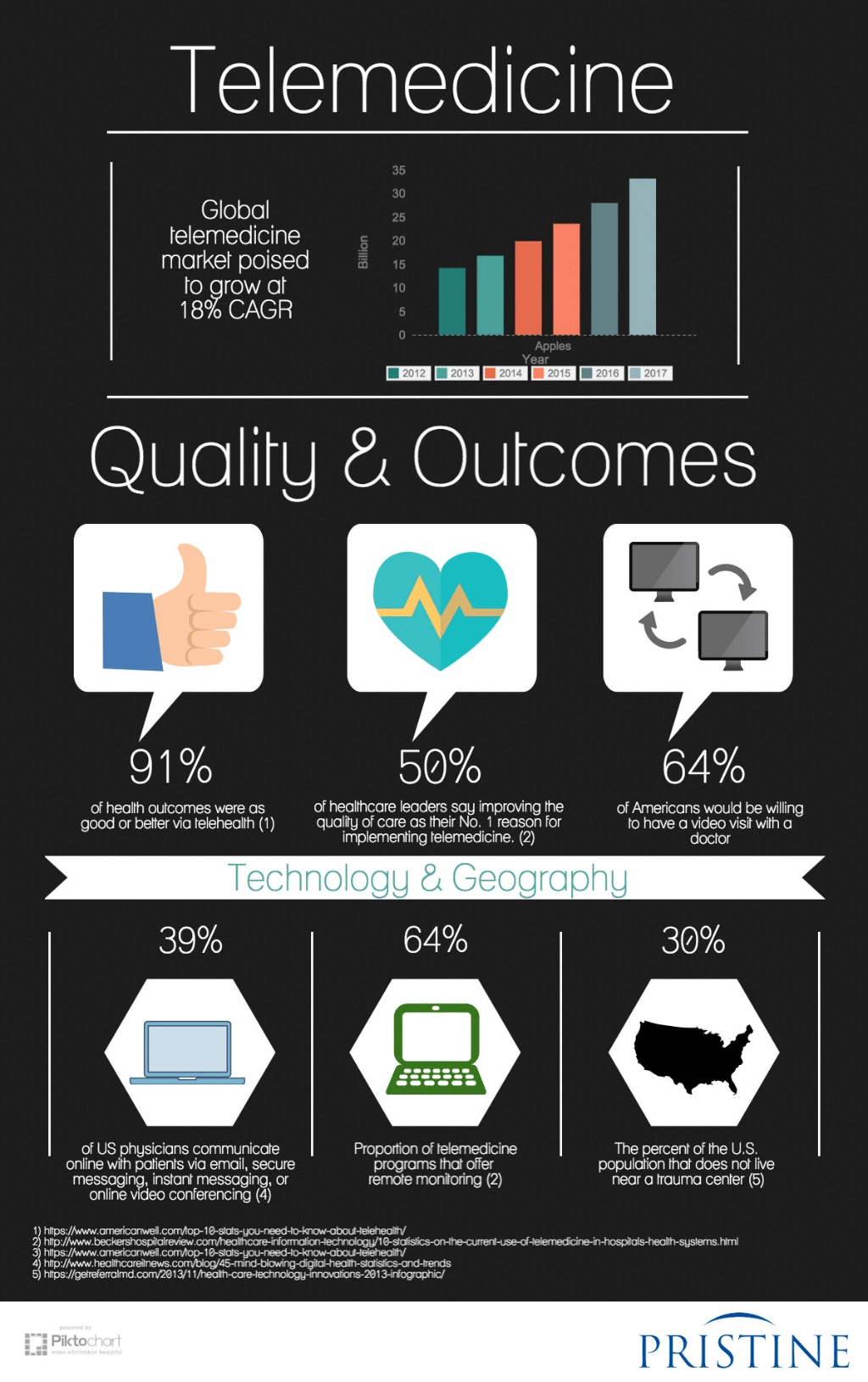
As Medstaff suggests that 90% of healthcare organisations have, or at least plan to have, some sort of telemedicine practice in place, perhaps it’s time to catch up with the competition and make telemedicine a part of your daily practice.
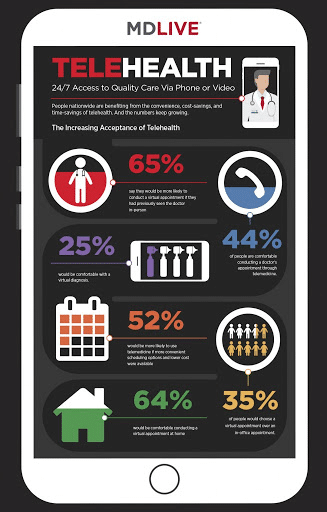
And it isn’t just medical practitioners who prefer using tech for treatment. eVisit says that 74% of patients are happy to use telecommunication to see a doctor, rather than visiting them face-to-face. This is especially important in today’s modern age of social distancing.
Telemedicine providers help connect physicians and other health care staff with patients. They enable healthcare professionals to deliver a range of telehealth services.
Of course, with Covid-19, many medical professionals are catching on to the idea of telemedicine. The knock-on effect of this being that there is also an influx of telemedicine providers. This can make it very confusing to know who to trust and who is merely latching on to the trend.
Source: Chiron Health
Telemedicine isn’t just a case of logging into a VoIP app and talking to patients. Or indeed, patients video calling a hospital and being able to talk to a doctor on demand. Telemedicine providers need to have special training and the right equipment. Training in telemedicine can take years. And with technology changing all the time, a provider must adapt to these changes too.
As the type of care that people need varies from situation to situation, it is vital to work with a telemedicine provider who knows what they are doing. Not one who has watched a quick online video and bought some second-hand equipment.
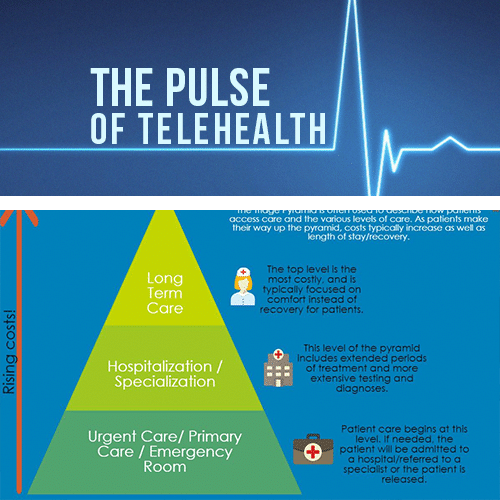
Source: MeMD
An orthopaedist maybe checking on the progress of a broken leg and talking to a patient that they have met before. An A&E nurse may be talking to a patient who lives in the mountains and has a shallow gash. Or a therapist may be assessing a patient’s behavioral health. So, it’s important to work with a telehealth provider who knows which equipment is needed for what kind of health care worker. As well as the kind of specialist way they can help you.
What is Telemedicine?
Officially born in the 1950s, telemedicine is a way of using technology to connect with patients who can’t be seen in person. After a lot of experimentation, it was originally created to connect health professionals with people who lived in remote places. However, after realising the benefits, it was soon used to help people in poorer areas who didn’t always have a high level of access to healthcare.

Source: sisgainmobileappdevelopment
After years of practice and modernisation, professionals have realised what huge value it has to the healthcare system. Thus, they are implementing it in hospitals, doctor’s surgeries, and clinics around the world.
Patients connect with clinicians, nurses, and various other types of health care workers using a screen to screen system. This could be through a VoIP phone system, or it could be done using webcams on computers. As 3.5 billion people own a smartphone worldwide, according to Bank My Cell, many people can also receive patient care through a mobile phone. Meaning an appointment can take place from anywhere. Something very beneficial for that self-isolating or social distancing due to coronavirus or other infectious diseases.
Types of care that can be provided through a communication device can range from a nurse checking on wound care, to a psychiatrist assessing a patient’s mental health and providing therapy sessions. It is cost-saving, safe, and modern. What’s more, it gives healthcare providers that much needed knowledge that is often missed out in training and educational courses.

Source: Vidyo
Depending on the type of care you want to provide, the place you work, and the number of people in your team, choosing the right provider will help you choose what type of telemedicine and equipment will work best for you.
Benefits of Telemedicine
Every practice has its good sides and bad sides. But this is a healthcare system that has many more positives than negatives.
The most obvious point is that it is taking advantage of the tech available. And not just tech that is available to medical professionals, or centres with specialist funding. In many countries, healthcare doesn’t get the funding it needs and for many people, they too don’t have the money to get vital patient care.
As an example, Flymedi tells us that the treatment of chemotherapy in the USA costs an average of $100,000. For many, this is unaffordable. Of course, telemedicine can’t provide chemotherapy. But it can provide access to medical professionals for counselling and follow-up sessions at a much cheaper rate. This could be critical to a patient’s mental health and wellbeing.

Source: American Hospital Association
In being able to access telemedicine services, all people need is a smartphone. So, this is medical help, and technology, that is available to many, rather than just those that can afford it. Not forgetting that many places still use outdated pieces of tech that sometimes provide inaccurate results and slow down the caring process.
Telehealth is also able to save healthcare providers and companies money in general, as there are no transportation costs, no childcare costs, and no cost of extra expensive equipment.
Another obvious advantage is the non-face-to-face contact that exists within providing telemedicine care to patients. In times of airborne pandemics, like Covid-19, this has been particularly important. But this is also very beneficial to people who are at high risk of vulnerability or have low immune systems. It is also a great system for people who live far away and don’t have access to hospitals nearby.
Other benefits include reduced waiting times, more time with each patient, and, with higher access to information, smarter and more in-depth decisions being made. Those who need access to specialists also have this opportunity, without having to travel long distances to talk to them.
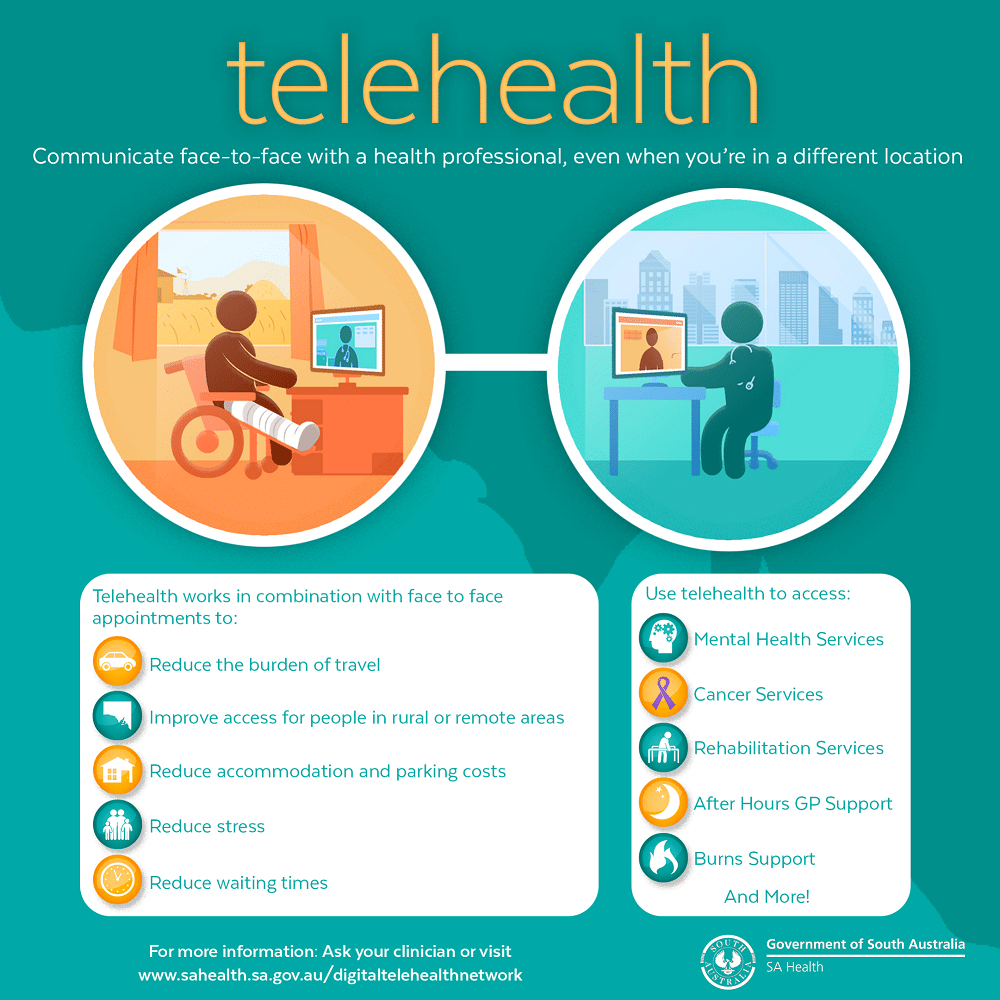
Source: SA Health
One of the biggest positives of telehealth, perhaps, is the result of overall improved public health. Having access to telemedicine means that people can see doctors more, are encouraged to take medication when required and can make appointments with physicians on demand if needs be.
There are personal benefits for the practitioner too. With extra time, the doctor is no longer burdened with high levels of work. Meaning stress and risk of burn-out is automatically reduced. Long commutes and long-distance travelling is also reduced. Meaningless environmental impact, while time and money are also saved.
This is not to say that telemedicine companies exist without cons. Residents in countries like the UK, France, and Israel are lucky enough to be able to experience free healthcare through their health systems. But for others, their health insurance may not cover the use of telemedicine. Such as those in the United States on Medicaid.
Furthermore, despite being at the forefront of technology, some technical restrictions come with only being able to communicate through a computer or phone. For example, the patient will not be able to receive a physical examination or as comprehensive mental health care and vital issues may get missed.

Source: Lean Forward
Despite these negative points, telemedicine still has many positive attributes, with a great impact on both patients and care providers alike.
Introduction to Telemedicine Providers
Before you invest any time at all into virtual care, you need to think about whether providing this type of care will be equal to, or more beneficial, to your patients than the in-person care they currently receive.
If you still want to go ahead, then it’s useful to consider these points.
When setting up an online care network, you must go with one that suits you and your needs. This can make the difference between a well-thought-out and dedicated practice, and one that isn’t too sure what they are doing.
It’s not just a case of picking a telehealth provider and hoping they are the right fit. Each medical worker will have a different need, and each service provider will have various strengths and weaknesses. A small practice will not have the same budget that a huge hospital will, for example.
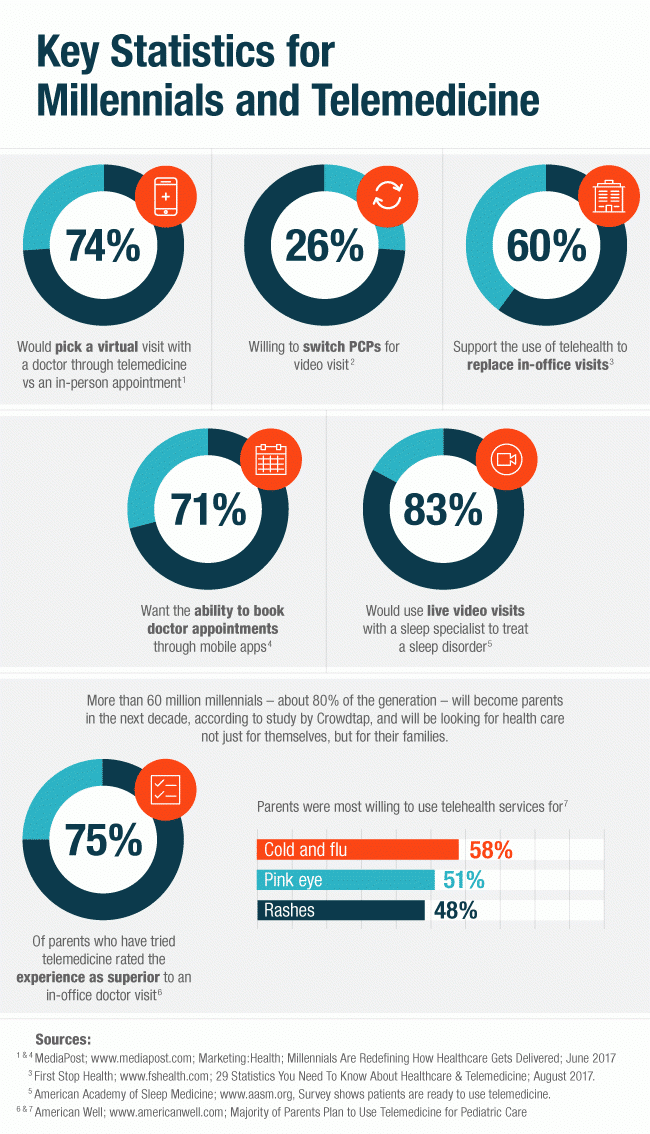
Source: Media Logic
You need to consider the specific needs of your patients and the specialisations you may have as a healthcare professional. Think about the problems you are trying to address and how virtual care will help with this. Use a telemedicine provider that aligns with these values and can provide you with your specific wants and needs. Make sure the technology fits with the service and that the telemedicine company you choose can deliver this.
Keep in mind that all your patients are different. This may seem like an obvious statement to make. But you don’t want to end up in a situation where you have invested a lot of money into a telehealth provider with the presumption that your patients will be able to instantly use the service. Therefore, you need to pick a provider that reflects on this.
Source: Bottom Line
Telemedicine companies need to provide you with a service that benefits patients of all abilities and ages. The best telemedicine providers will be honest and work with you to provide what is best for you and your patients. Once you have figured out which devices people have access to and what their needs are, then you can work with a telehealth company to choose a telemedicine platform, and go from there.
This will, of course, be easier for smaller firms, but even if you are working on a large scale, you can figure out what your specialist departments are, which areas would benefit the most from this service, what type of patient you are trying to reach/help, and where there is a gap in service.
You also need to consider what the follow up will be for patients and how a telehealth provider will help you deal with this. As well as this, it will affect the workflow of your staff.

Source: Incremental Healthcare
Types of Telemedicine Providers
More and more businesses are getting involved in selling telehealth. Meaning there are a plethora of options from which you can choose. However, whichever one of the telemedicine companies you decide to go with, consider which has the best-suited options for your needs.
There are four main types of telemedicine out there. Think about how each one fits with your practice and the benefit it will have for your patients.
-
Live Real-Time Video
This kind of virtual visit is the closest that a person can get to a real-life doctor’s appointment. The patient can tell the practitioner their problems and the healthcare provider can try to find a solution. Just like when going for a regular visit to the doctor. The only difference is, everything gets done virtually and neither person has to leave their home.
Sometimes a patient will get their own doctor, sometimes they won’t. This depends on circumstance and problem. Either way, systems make sure to follow strict patient confidentiality. This practice is also known as interactive medicine.

Source: General Devices
-
Remote Patient Monitoring
Otherwise known as RPM, this type of telemedicine allows data to be collected, then electronically transferred from healthcare workers in one location to another.
It also allows healthcare professionals to monitor patients when they are at home. They collect data by using technology and teach patients a level of self-care that allows them to gather data. Such as learning how to take blood pressure, blood sugar level, or temperature. This practice is already used with hospital staff as it reduces readmission rates.
-
Store and Forward and Transmission
An excellent way of enabling staff to work together from anywhere, this type of telemedicine provider allows health care workers to share patient information with different practitioners in different locations.
Source: Vivify Health
It helps health professionals to make rapid and accurate decisions, as they have access to patients’ pre-recorded histories, including any videos, photos, or diagnostic imaging files. The information is then used by a specialist to make an evaluation. This is often done out of real-time. This type of telemedicine provider is great for giving primary care to patients in far-out geographical locations. It provides them with information on specialist care without having to see the patient in person.
-
Mobile Health Platform
As more people take health into their own hands by using tech to research and monitor problems, Mobile Health Platforms, otherwise known as mHealth, are taking advantage. Think, smartwatches, daily step counts on phones, etc.
Healthcare providers and policymakers use this information to make decisions and determine treatments. They also use the data to look at the bigger picture in health by assessing trends and evaluating larger health issues. All through the information provided via personal devices. Sometimes, this data is also used to make decisions on public health issues, such as encouraging people to walk more, etc.
Source: The Sextant Group
Think about how these types of telemedicine providers and telehealth services may reflect on your requirements and the needs of your patients. Consider how they will fit in with your practice.
What to Look For in a Telemedicine Provider
When hunting for a telehealth company that works with your medicare needs, you need to be aware of certain points to keep in mind. If you are unsure, here are five aspects of telemedicine services to keep in mind during your search:
- Does the program have a user-friendly design? – When medical staff decides to go virtual, they tend to have some sort of training so they are up to date with all the tech they use. Patients, however, do not have this opportunity. So, it’s important to make sure whichever design you choose is friendly on all sides. That’s including when it comes to any patient portal.

Source: Capterra
It needs to be accessible to people who may have no understanding of tech at all, as well as those who are experts in the field. That means people of all ages, all abilities, and all backgrounds. Consider things like language barriers or sound and vision issues when it comes to video visits. As well as the income of some of your patients. For example, you may have patients that are visually impaired and also low income. Will they be able to see you when you are talking and do they have access to a larger screen? If not, you need to choose a virtual care platform to compensate.
Always think about your patients, their needs, and your specialty. The best way to see if the design is suitable is to ask patients to sample it and see if it works for them. Make sure that any colleagues using the system will also feel comfortable with it.
- Does it integrate well? – The point of investing in telemedicine is that it makes the lives of you and your patients easier. So, it’s important that you choose a telehealth provider that integrates well with your working practice. You need a system that allows you to easily access files, talk to patients, and manage multiple applications.

Source: General- devices
Choosing the right platform will allow you to keep on top of your schedule, patient files, and records. Making your workflow much easier and allowing you to efficiently meet the needs of your patients.
- Work out how it fits with your practice – Every organisation works differently, has different specialties, and varied patient needs. Meaning that whichever design you choose has to fit around your requirements. As you may need to provide specialty care, you should ensure that whatever system you choose is customizable. Keep in mind, though, that video calls may not be best suited to urgent care or triage.
Again, consider what works best for your patients, too, and the type of treatment they would like to receive. Do they prefer video chats or telephone chats? A lot of mental health providers also do write chats, so that may be something you also want to consider.

Source: Hin
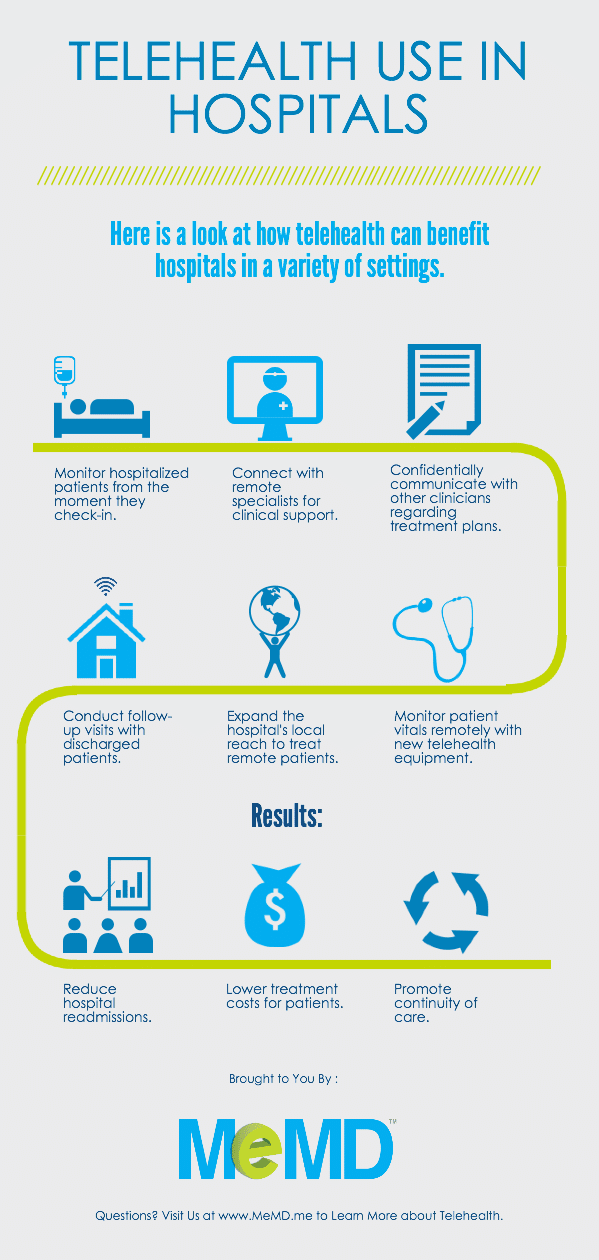
- How does it fit with specialty care? – Whether this is something you practice every day or a one-off situation, the platform you use should also be prepped with a way to handle specialty care. Lots of patients actually don’t have access to specialty care because of a lack of funds or a lack of experts in their geographical area. So, why not provide this for those patients who need it?
If you aren’t able to provide these sorts of healthcare services yourself, think about integrating communications with a specialist provider who can give this care.
Source: MeMD
- Can you use it to collect data analytics? – You may not think it, but collecting data analytics is a key part of improving medical services. Meaning that if you can use a program that does this job for you, you are saving time and money, while also improving the future of your service. It helps you figure out what works, what doesn’t, and what’s somewhere in between.
What’s more, having instant access to patient’s data means they won’t be waiting around to find out about their own information.
Keeping these points in mind will help you to choose the telemedicine provider that is best suited to you.

Source: Chiron Health
Top Telemedicine Providers
After reading through all this information, you may have decided that you are ready to invest with a telemedicine provider. However, starting can be a little intimidating. You have all the knowledge of what to look for from a telemedicine company, but you don’t quite know which companies to trust.
Here are a few suggestions of the top telemedicine providers to get you started.
Beam – This telemedicine provider is aimed at allowing primary caregivers to reimburse claims for online visits with little or no interaction from patients or doctors. It is free to use for physicians and works by using an end-to-end solution.
Nurtrimedy – This start-up works alongside clinical dietitians to deliver nutritional care outside of a hospital environment. It works alongside medtech and biotech to help with over 50 conditions. Part of its appeal is that it works on a personal level to find a program that works on an individual basis.

Source: sisgainmobileappdevelopment
Zipnosis – This provider treats patients with common health conditions. They offer virtual care and engage with patients to offer a flexible service. Zipnosis has customised modalities.
GYANT – This telehealth provider analyses patient medical histories to help them gain access to healthcare. It offers help in minutes. GYANT’s user experience is highly rated amongst patients.
Psyalive – This allows patients and psychologists to connect through video conferencing using their native language. Thanks to effective algorithms, suitable matches are made based on the patient’s requirements. Psyalive helps companies provide a service between corporations and employees.
Source: Medgadget
Conclusion
When choosing a telemedicine provider, it’s important to weigh up options. Different providers will have different specialisations, and this should be key in making your decision.
There is also the consideration of how each provider integrates with your practice. Would real-time video or RPM work better? Perhaps Store and Forward and Transmission will be more effective. Or maybe mHealth is more apt for your patient base.
Whatever you choose, make sure to pick an option that suits both the needs of your daily practice and the requirements of your patients. A nurse practitioner covering rural areas would need something different from a therapist providing remote care. In doing this, you will create a smooth workflow, improve health, and find helpful solutions for those to whom you provide care.
Get details on the security and trust built into RingCentral products and services.Download the white paper
Updated Jan 16, 2023



