Over the last few years, there’s been a lot of talk about the changes we’re seeing in healthcare. The revolution in big data has been particularly hyped up, and with some justification. It isn’t just about collecting large quantities of data, but knowing how to analyse it. Doing so effectively gives more insight into patients’ health and how lifestyle or genetic factors might affect it. But the technological transformation we’re seeing doesn’t stop there. Telemedicine also appears set to change the face of healthcare provision and perhaps the health system as a whole.
Telemedicine has been around for a while, although take-up remained fairly modest for quite a long time. Until, that is, the Covid-19 pandemic struck. With social distancing measures in place across the world and doctors trying to limit face-to-face contact with patients, more and more have come to use telemedicine apps. This means that they can hold consultations with patients and offer primary care, without the need to see them in person. Even assuming a Coronavirus vaccine arrives in the not-too-distant future, it is likely that telemedicine is here to stay. Especially as both healthcare professionals and patients alike get more accustomed to using it.

The recent rise of telemedicine, though boosted considerably by the pandemic, chimes with other aspects of our daily lives. We’ve now become increasingly accustomed to video calls and video conferencing, and the way we work has been transformed along with our everyday routines – keeping in touch with clients and colleagues in far-flung locations, as well as friends and family.
It seems natural, then, that even when the pandemic is over, telemedicine will most likely continue to enjoy a bright future within the healthcare system. It allows us to have a quick and convenient consultation, without the hassle of having to drag ourselves to a doctor’s surgery or clinic.
It seems natural, then, that even when the pandemic is over, telemedicine will most likely continue to enjoy a bright future within the healthcare system. Click To Tweet

So what exactly is telemedicine? What are the prospects for telemedicine in the UK? What are its advantages and its disadvantages? In this guide, we’ll give you an in-depth overview of what telemedicine is (and telehealth more generally) and how it might transform the way we receive healthcare in the coming years. We’ll provide a concise definition of what telemedicine is and explore its history in some detail. Then, we’ll look at the benefits and potential drawbacks of telemedicine, as well as the different types of telehealth services and the terminology used. Read on to find out more.
What is Telemedicine?
In short, telemedicine is the term given to remote health care delivery and consultation given to patients at a distance.

For example, via the internet and video chat apps. As video chat becomes more and more commonplace, a lot of healthcare providers are looking to telehealth methods to help them make tight budgets stretch that bit further.
Patients themselves, it appears, are becoming increasingly accustomed to the idea, too, after some initial uncertainty. As we’ve discussed, the Covid-19 pandemic has led to a sudden increase in remote consultations, as doctors look to restrict the use of face-to-face meetings with patients.
Telemedicine allows patients and doctors to converse with one another remotely, wherever they happen to be. That’s as long as they have access to a sufficiently reliable internet connection. However, it offers more than just standard video calls. Doctors and patients can share different types of information using telemedicine apps, including blood pressure test results and readings from medical devices.
Patients have come to expect – as technology has changed their own everyday lives – that health care delivery should do likewise. Of course, telemedicine is not a complete substitute for face-to-face consultations or clinical services; there will be instances where health professionals will need to see patients in person. Nevertheless, it is a convenient option for quick check-ups, and so on.

There are different types of telemedicine, which is something worth bearing in mind. There are three main types in particular:
- Interactive medicine (where patients and doctors communicate with each other in real-time),
- Store and forward (where providers are permitted to share patient health information with physicians elsewhere)
- Remote patient monitoring (where mobile medical devices are used to collect data which is then used by remote caregivers to monitor patients and health outcomes).
Interactive medicine is the kind of telemedicine that most patients are familiar with. There are several mobile apps that they can use to obtain a remote consultation with a physician.
As we’ve just noted, there are different ways of providing remote telemedicine care. Most commonly, patients participate in a video call with a doctor and discuss whatever medical issues they need to discuss. Telemedicine apps are held to stringent standards of data protection and security so that patients’ privacy is safeguarded.
Some kinds of telemedicine services, however, may involve providing patients with portable kits and devices to monitor their condition. Telemedicine may also take the form of video conferencing and data storage and sharing. It’s all a matter of what the patient needs and which particular method might best suit their individual medical care.
Telemedicine is now commonly used in the treatment of a wide range of medical conditions. These include to give just a few examples of telemedicine uses relevant here:
- Asthma and respiratory infections
- Cold and flu
- Sprains and strains
- Arthritis
- Bronchitis
In addition, surgeons may use telemedicine apps to catch up with patients following an operation to check their post-op condition. By the same token, an oncologist might use telemedicine to talk a patient through their test results and treatment plan. Calls like this can also be done over the phone, of course, but having video as well as audio helps provide patients with extra reassurance. That’s as well as allowing them to demonstrate certain physical manifestations of whatever condition they’re suffering from.

Furthermore, the type of telemedicine available will depend on the nature of the healthcare provider. Some private healthcare firms might offer telemedicine solutions for certain types of consultations, for instance, whereas others might be excluded.
If you’re unsure of what telemedicine options are available to you, it’s a good idea to speak to your doctor (or your insurer if you’re in the USA and covered by Medicare or Medicaid, for instance) for further information. You can also ask them for more information about the relevant regulations and security measures in place. It goes without saying that your confidentiality and privacy should be a consideration of the utmost importance. It’s always worth seeking out more details on the subject, therefore, if only for your own peace of mind.
Definition of Telemedicine
Given the rapidity of the recent growth we’ve seen in telemedicine, and the plethora of different services offered via telemedicine apps, there is – perhaps inevitably – some uncertainty about what precise telemedicine definition might apply in specific circumstances. The term ‘telemedicine’ is, as we’ve alluded to, used quite widely to cover a broad range of different functions and services.
Telemedicine companies themselves may sometimes use the term a little loosely. That doesn’t always make it easy for patients (as laypeople) to understand exactly what is meant by it. Let’s look more closely at how we might define telemedicine and hopefully dispel a lot of the opacity surrounding the subject. That way, we can ascertain the correct telemedicine meaning.
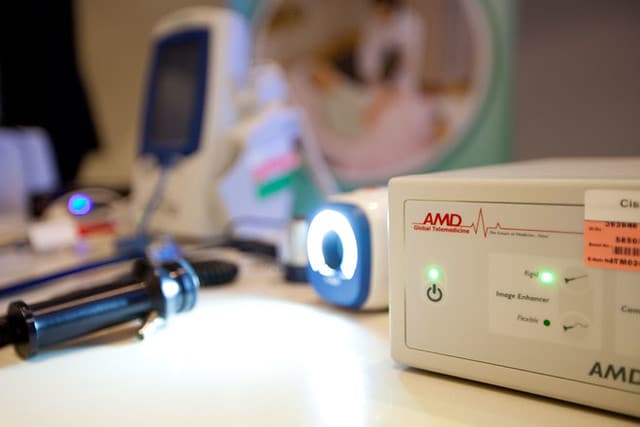
There is particular confusion around the use of ‘telemedicine’ and ‘telehealth’. These days, the two are increasingly used interchangeably, essentially as synonyms of one another. However, this can add to the confusion, and there are differences between the two which it’s important to bear in mind.
Telehealth, to be more precise, is an umbrella term used to encompass a wider set of healthcare solutions utilising information technology (IT). Telemedicine can be placed under this umbrella, but the term itself is more constricted in its meaning. Let’s take a closer look into the matter and hopefully clear up the confusion and uncertainty.

Telemedicine is defined by the World Health Organisation as “healing from a distance”. In other words, the remote provision of healthcare to patients. This would include, then, the use of telecommunications technology (such as video-based apps) in providing treatment or diagnosis to a patient remotely. In addition, remote imaging or video consultation would also come under the banner of telemedicine.
But what is telehealth? In short, telehealth is used to denote the use of information and telecommunications technologies to provide and support all of the following:
- Long-distance healthcare provision
- Public health measures
- General health education
- More specific medical education
- Administrative functions
Evidently, this is a far wider remit than that of telemedicine, although it would also cover the latter. The fact that supporting functions are also included in the definition of telehealth underlines this. It means that remote administrative meetings or video conferences among healthcare professionals might also serve as good examples of telehealth.
Clearly, telehealth and telemedicine definitions continue to be debated and contested within the healthcare sector. The media, as we discussed earlier, has a tendency to use both terms interchangeably, and as a result, patients do as well. In our discussion here, when discussing telemedicine, we will do so by this particular term to minimise the risk of any further confusion.
Nevertheless, if you’re an ordinary patient, i.e. a layperson, and you find yourself using ‘telehealth’ in discussion with a healthcare professional, they’ll know what you mean by it. Using the exact terminology isn’t necessarily the be-all and end-all.
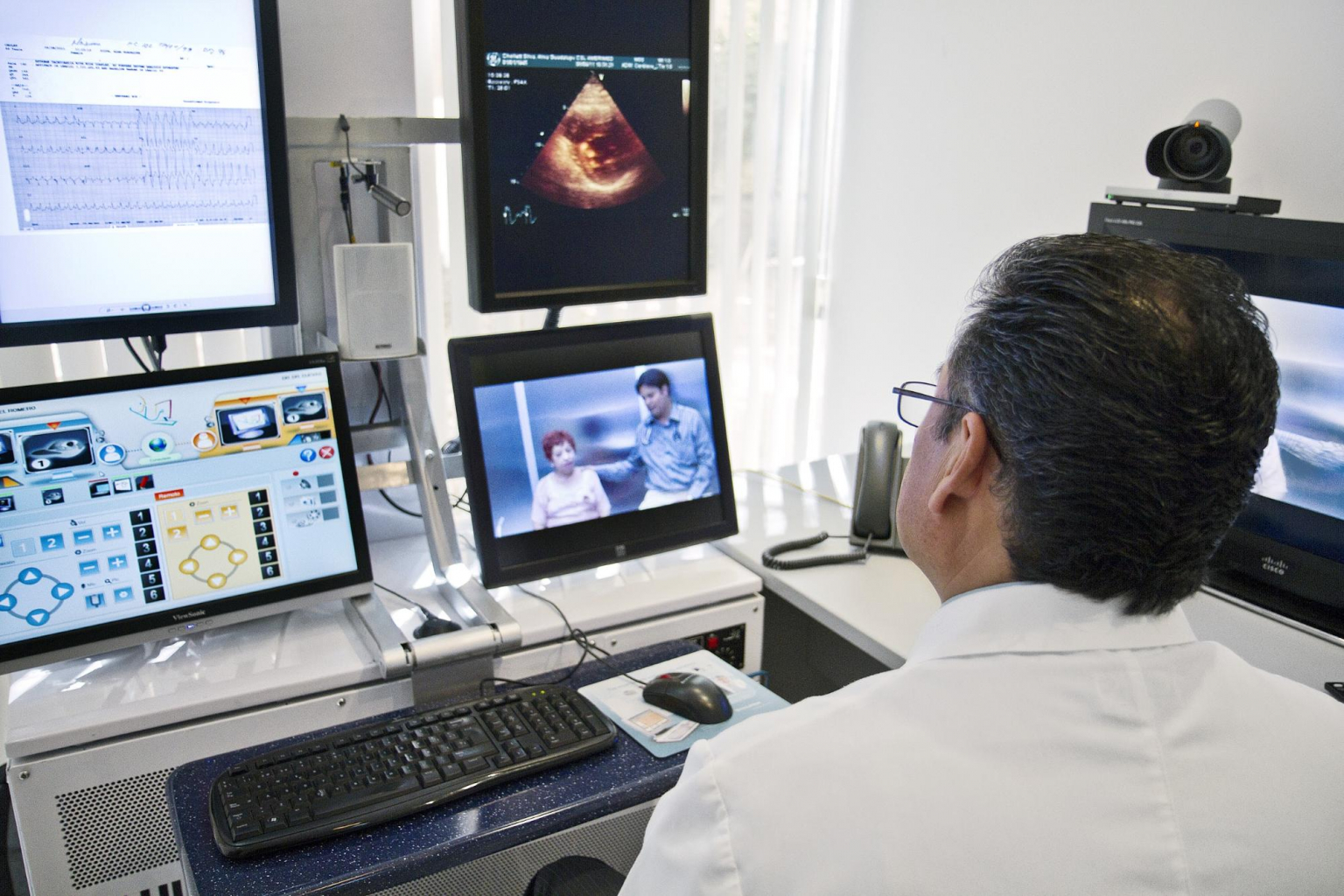
The likelihood is that as telemedicine continues to involve, this term will itself come to encompass a wider range of healthcare treatments and services. As such the boundary between telemedicine and telehealth will perhaps become rather more fluid than it has been hitherto.
For everyday patients, people who don’t generally keep up with developments in terms of the minutiae of healthcare provision, it may be quite easy to be confused by the terminology. This is something that telemedicine companies and physicians will hopefully be mindful of, and take into account.
Any patients who find themselves overwhelmed and confused by the varying, sometimes inconsistent, uses of different terms can always approach their doctor or search online (using reputable sources such as the NHS website) for further clarification.
History of Telemedicine
For all the recent hype about telemedicine platforms, you could be forgiven for thinking it’s a brand new phenomenon. It may seem like it’s emerged out of nowhere in the last decade or so. In actual fact, however, telemedicine technology has a heritage stretching back much further.
For well over half a century, healthcare providers and doctors have been experimenting with different types of remote service provision. It’s only in the last few years that this has flourished into telemedicine as we understand it today. So, let’s take a quick look at this history and learn how telemedicine has got to where it is now.
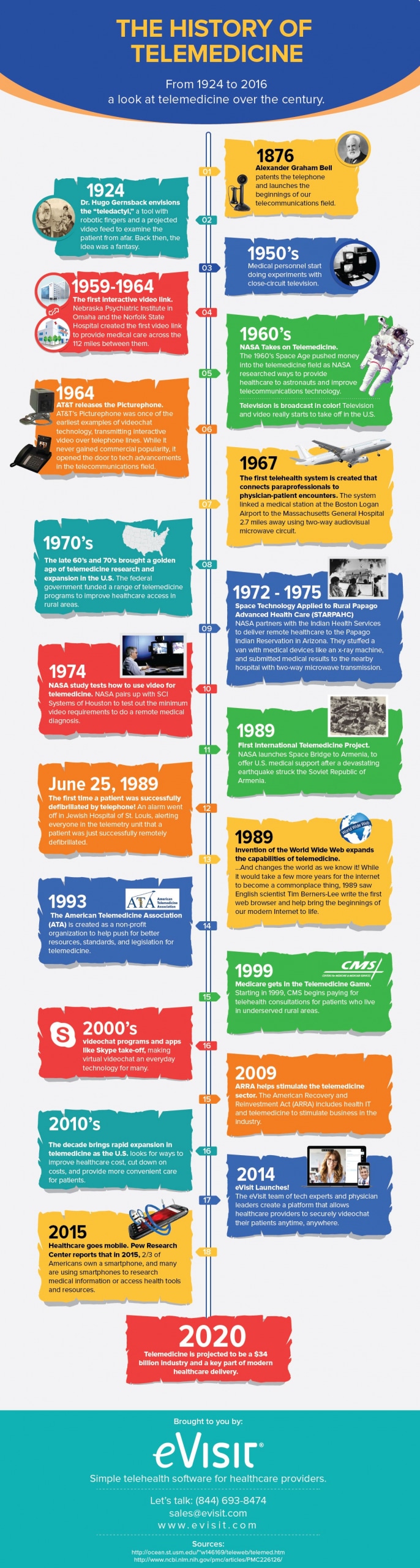
First, to understand this long heritage, we have to go back to the very origins of telecommunications technology. The rise of telecommunications began in the late 19th century. That was when technologies including the telephone (invented by Alexander Graham Bell in 1876) and the radio (pioneered by the likes of Heinrich Hertz and Guglielmo Marconi in the 1880s and 1890s), along with others such as the telegraph, emerged onto the scene.
Mass communications grew rapidly during the 19th century, with the advent of the railways bringing national daily newspapers into large-scale circulation. That constituted a coherent general public for the first time and created demand for more new forms of communication.
After the turn of the century, these new technologies were starting to be put to a range of new and inventive uses – including medical ones. This had been presaged by a report which appeared in the leading medical journal, The Lancet, in 1879. It had speculated on how the telephone might help to cut down the number of unnecessary office visits. This was an insight that would be carried forward in the following years. If the telephone and other such communications technologies could help us avoid making visits to offices that we didn’t need to make, what other uses might it be put to?
Of course, there were rather more unorthodox attempts at technological innovation as well. In 1925, for example, Hugo Gernsback – an inventor originally from Luxembourg – hypothesised the ‘teledactyl’. This was a peculiar tool that would have remotely examined patients using radio technology while relaying a video feed to an onlooking doctor. This gadget never came to actual fruition – which, perhaps, is just as well. It did, however, help plant the seed for remote consultations with patients via video link. Albeit, it took many more years for this to become an everyday reality.
By the 1950s, more recognisable forms of telemedicine were beginning to take shape. Around this time, two health centres in Pennsylvania in the United States used telephone technology to exchange radiologic images. This was subsequently developed into a ‘teleradiology’ system used by Canadian physicians in the Montreal area.
Another major advance came in 1959, when the University of Nebraska used a two-way interactive television system to transmit images of neurological examinations to students across campus. Five years later, a link with Nebraska’s Norfolk State Hospital was established. The hospital was 112 miles away from the university campus, but the link could be used to provide various healthcare services.

When these early forms of telemedicine were still in their infancy, they were primarily used to reach patients living in remote rural areas of North America. Those places, after all, were lacking in medical facilities and practitioners.
However, it wasn’t long before healthcare providers and government bodies began to recognise the wider potential of this new technology. Especially in allowing them to address health concerns among marginalised urban populations. They themselves were often struggling to obtain accessible consultation and treatment. The potential of telemedicine, too, was spotted in terms of cutting down on waiting times by facilitating easier sharing of patient records and test results.
As a result, telemedicine received a huge investment boost from the US government. From bodies including Nasa, the Department of Defense, the Health and Human Sciences Department, and the Public Health Department. These finances spurred further innovations in telemedicine and saw the technology evolve rapidly during the 1960s and ‘70s.
One early application of a kind of telemedicine was the use of voice radio channels by fire departments. They used those to transmit electro-cardiac rhythm signals from sites where emergencies had occurred to local hospitals. This thus allowed physicians at the hospitals to track patients’ vital signs at a crucially important period.

Another telemedicine project from this time was Space Technology Applied to Rural Papago Advanced Health Care (STARPAHC). More than just an alphabet soup, this partnership between Nasa and Indian Health Services developed remote medical services that could be provided both to native American people living on the Papago reservation and Nasa astronauts on their space missions.
While a relative niche affair projects like STARPAHC again helped to spur further discoveries in the telemedicine field. All the while teaching practitioners new lessons about how the technology might be used to provide medical services and simulate virtual visits to people in all manner of locations.
In more recent years, telemedicine and telehealth have proliferated to cover a wide range of technologies and services. Telemedicine apps are of course being used increasingly widely. But other modern healthcare technologies also take their cue from this history of telemedicine.
Fitness wearables, for example, such as heart rate monitors, smartwatches, and wristbands, monitor and display health data in real-time. Even mobile phones routinely include their own telemedicine apps, tracking users’ daily step counts. With such devices – along with laptops and tablets – in such widespread use, patients’ accessibility to remote telemedicine medical services is easier today than it’s ever been. It looks set to increase further over the next few years, too.

Benefits of Telemedicine
The potential benefits of telemedicine have been the subject of much hype and discussion over the last decade or so. We’ve already discussed how the Covid-19 pandemic has forced doctors to provide more services remotely. That’s as they seek to keep as many patients as possible out of clinics and surgeries (and away from crowded, cramped waiting rooms where the virus can easily spread).
There is little doubt that telemedicine is here to stay. But it’s worth taking a closer look at the benefits it might potentially have, and why both patients and telemedicine companies might benefit from the increased and expanded rollout of telemedicine services.
The most immediate benefit of telemedicine is that it opens up the potential to provide patients with convenient and easily accessible healthcare, allowing for better all-round patient experience. Obviously, some patients – particularly those who are sick or have suffered some sort of physical injury – may have limited mobility, in which case getting to surgery, doctor’s office, clinic, or hospital would be inconvenient for them. Likewise, doctors are not always available to make home visits (their time is at a premium and they have a lot of patients to deal with) so telemedicine helps both parties to save unnecessary time and effort.
It also creates the possibility of providing healthcare to people who might be lacking in healthcare facilities in their immediate local area. We’ve just discussed how smartphones, laptops, tablets and other such devices are now owned by the overwhelming majority of people in countries like the UK. They’re also a staple of a substantial proportion of the population in less affluent countries.
Telemedicine allows people who perhaps don’t have a clinic or surgery near to them to obtain a consultation with a physician, whereas before they may not have been able to do so.
Thanks to telemedicine, patients can also access treatment from niche healthcare specialists (who are, by definition, not always so easy to access as general practitioners). If patients need to see a physician specialising in a less common kind of illness or condition – for example, rare types of cancer – they can do so via video link through a telemedicine app or service.
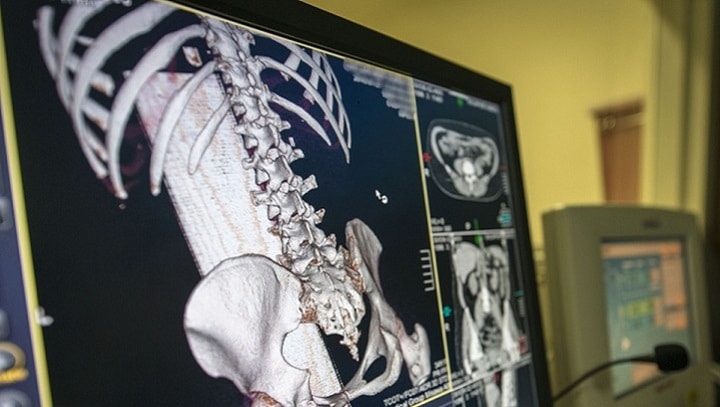
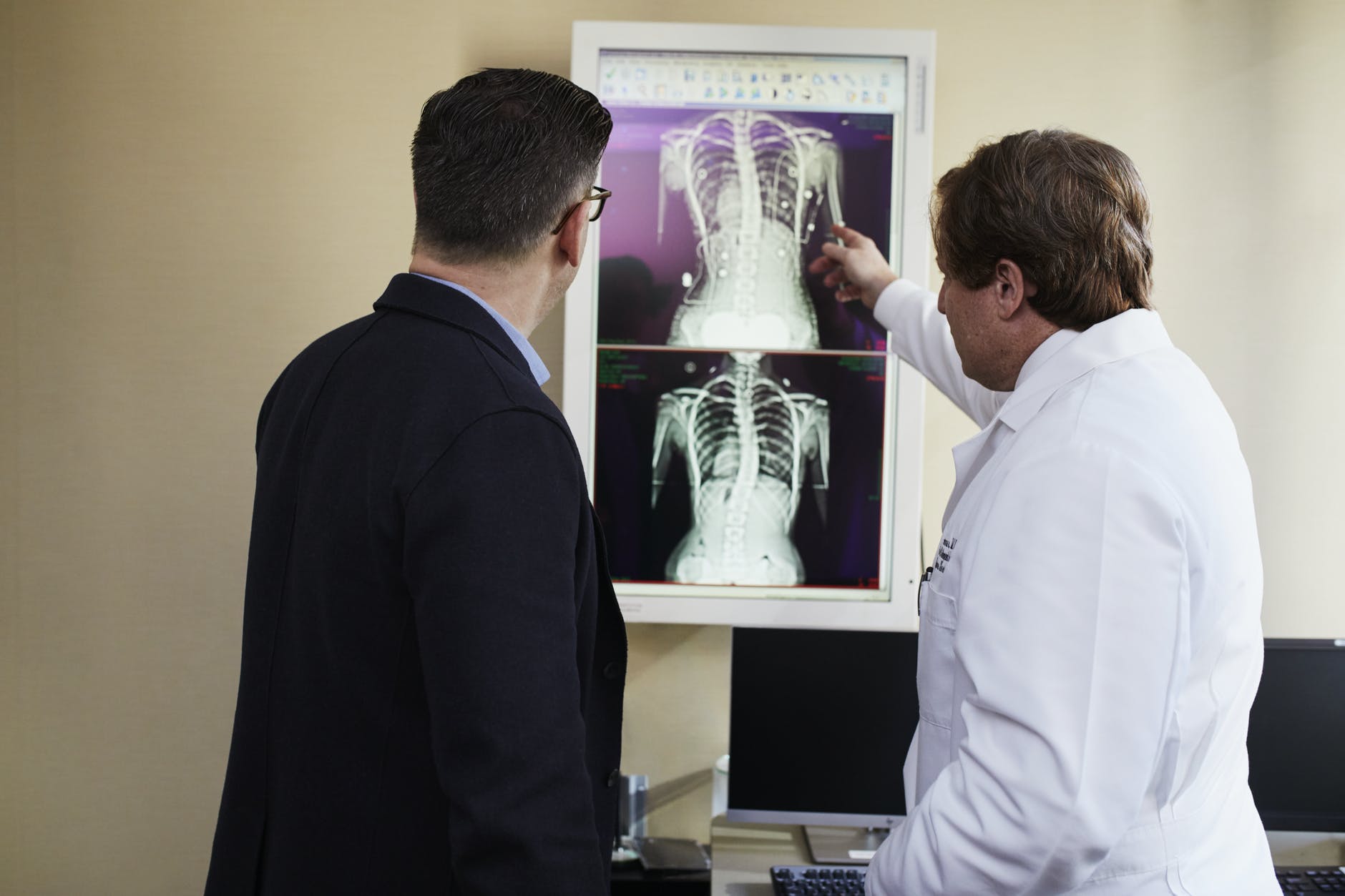
In addition, smaller hospitals that lack certain facilities can use their own telecommunications services to effectively outsource particular treatments or diagnostics. For example, processing test results or inspecting X-rays.
Another advantage of telemedicine is that it gives patients more of a direct say in the way they’re treated. Many patients experience frustration when they perceive that their physicians aren’t paying much attention to what they’re being told. Others simply avoid or skip doctors’ appointments, with many people apprehensive about them for a variety of reasons.
Telemedicine helps patients to connect with physicians on a more regular basis, thus allowing patients to forge better relationships with their doctors. This also gives them more incentive to attend check-ups by taking a lot of the hassle out of it. They can discuss matters with their doctors from home, rather than having to venture out to see them in person.

Furthermore, telemedicine can help healthcare budgets reach further. We’ve pointed out already how a lot of healthcare providers can be somewhat strapped for cash, perhaps due to financial constraints imposed by governments. This can leave them struggling to fund certain types of service, requiring them to make changes elsewhere in order to free up financial resources.
Telemedicine could help to resolve such problems by making the provision of healthcare more efficient, allowing health bodies to reallocate funding elsewhere. Funding which is urgently needed for other purposes may, therefore, be more readily available, leading to better outcomes for patients across the board. This is one reason why we should expect telemedicine NHS services to expand quite substantially.
Above all, though, the biggest potential benefit of telemedicine is that it could be used to provide patients with better care – thus enhancing life quality as well as saving lives. With telemedicine, it’s simple for patients and physicians alike to check in with one another and discuss how the treatment is proceeding, future treatment options, and so on.
Telemedicine is being used for increasingly advanced types of treatment, making it easier for patients to access while driving up standards of patient care. These aren’t just marginal advantages but could go on to enrich many lives by ensuring that patients get the right kind of care where they need it.

With consumer technology so widely available – most of us rarely go anywhere without our smartphone in tow, for instance – it makes sense to use it so that patients can be reached with greater ease. It’s already natural for us to use our phones for the purposes of video calls, and so it’s not a great shock to the system to see medical consultations being conducted remotely.
It may take some time yet for all patients (particularly those of older age groups) to get properly accustomed to the idea. But telemedicine is, nevertheless, unlikely to disappear, and could represent the biggest advance in healthcare provision for many years. The benefits of telehealth are, likewise, already widely recognised by professionals.
Types of Telemedicine
So, we’ve already noted that there are several different types of telemedicine. It’s not just about the video consultations with doctors you might have had yourself, or perhaps seen on TV. Telemedicine is quite a broad term covering several different technologies, while telehealth is even broader than that.

In the years ahead, as telemedicine continues to develop and grow in popularity, it’s quite likely that new telemedicine services and technologies will appear. Here, we’ll take a deeper look at the various current types of telemedicine and what they do.
1. Store-and-forward
Store-and-forward telemedicine, also known as asynchronous telemedicine, is a method which medical practitioners use to share patient information remotely. These records could include, for example:
-
- Videos
- Test results
- Imaging studies
- Other information relevant to patient care
While this might just sound a bit like email, it’s different. Mainly because there are much more stringent security controls built in to ensure that a medical record or other patient information is kept private.

There are various advantages to both practitioners and patients of using store-and-forward or asynchronous telemedicine. The most obvious of these is its efficiency. It’s much easier for medical specialists to send important patient information to one another so that the nature of ailments can be determined quicker, thus allowing for more efficient care.
It helps to facilitate close collaboration among colleagues in different locations, as information and patient data can be shared around and reviewed much more easily. This works in much the same way as a team collaboration solution that you may use for your work.
Store-and-forward telemedicine platforms also allow different healthcare providers in different locations to exchange information quickly and securely. So, if you’re a patient who’s lived overseas and your records need to be obtained from a foreign healthcare provider, store-and-forward makes this fairly simple. It is commonly used in a range of medical fields, including radiology, ophthalmology, dermatology, and pathology.

2. Remote monitoring
Remote monitoring is fairly self-explanatory – as the name indicates, it involves using various technological devices to consult with and monitor patients remotely. It may also be referred to as self-monitoring or self-testing and allows healthcare practitioners to keep track of patients’ health at a distance. This is why it is widely used in the monitoring of a range of chronic illnesses, including asthma, diabetes, and cardiovascular disease.
Patients with diabetes, for instance, can use remote monitoring to keep doctors updated about their glucose levels, as well as allowing for patients living in social care facilities to have their health monitored. It enables people to test themselves in the privacy of their own homes and then relay the data to their physicians. It goes without saying that this can be much easier than heading out to surgery, clinic, or hospital to be tested for a particular ailment.
However, it is important to remember that patients are only laypeople, and there may, therefore, be a risk that they don’t test themselves in the right way. This would render the results of said test, if there are any, unreliable or ineffective. This is a matter for telemedicine companies and healthcare providers in general. They must be clear in their instructions to patients undertaking remote monitoring. Nevertheless, it appears that remote monitoring produces results that are about as accurate as standard testing undertaken by medical professionals.

3. Real-time telemedicine
This is the type of telemedicine that perhaps most patients (even those who haven’t used it) are familiar with, or at least aware of. It offers patients, among other things, a convenient way to arrange a consultation with a medical specialist so that their condition can be discussed. It spares them the trouble of having to arrange an in-person visit, which for people with multiple conditions can be a hassle. A typical telemedicine app will offer the option of arranging real-time video consultations with doctors.
Real-time telemedicine involves the use of video conferencing software to hold consultations with patients. As internet technology has advanced so much in recent decades, it’s now possible to have reliable remote video consultations online.
Perhaps the main difference between real-time telemedicine and other types of telemedicine is that the latter is often used to complement in-person visits to the doctor or the hospital. Real-time telemedicine is commonly used to replace the need for a face-to-face visit. Although obviously these may be needed where further treatment is required.
Because it’s so convenient, real-time telemedicine is used in a wide variety of situations. They include:
- Primary and urgent care
- Managing chronic or long-term conditions
- Follow-up discussions.
While real-time telemedicine consultations work in quite a similar way to conversations held via standard video apps, they’re not the same thing. Given the sensitivity of the matters being discussed, telemedicine apps are subject to much tougher security requirements so that patients’ sensitive information is kept safely under lock and key.
As well as convenience, there are numerous other advantages of real-time telemedicine software. It is also very cost-effective (allowing, as we discussed earlier, healthcare budgets to potentially stretch further) and enables enhanced patient satisfaction. Continually trooping out to see doctors face-to-face about ongoing health conditions may be inconvenient, even for patients without mobility issues. Remote monitoring saves them from having to arrange continual in-person appointments, which is much easier for those with busy schedules (and, for example, young children to look after).
There are other types of real-time telemedicine beyond standard video consultations with a GP. These include teleneuropsychology, which involves neuropsychological assessments undertaken to ascertain whether a patient has a cognitive disorder or other mental health issues. There’s also telenursing, where remote consultations are undertaken to determine a diagnosis or monitor patient symptoms for relatively minor ailments.
In addition, telepharmacy provides patients with remote pharmacy advice, while telerehabilitation is used to oversee clinical assessment and therapy for patients in need of physical rehabilitation.

Whichever type of telemedicine you need as a patient, your healthcare provider, and telemedicine companies should be on hand to help guide you to the right solution. Each different type of telemedicine has its place, and as the technology continues to expand, we will no doubt see new telemedicine services appear.
The key objective of telemedicine is to ensure that patients receive the care they need, to the appropriate standard, in a setting that’s as convenient as possible for them. We can expect that, in the coming years, telemedicine will continue to improve the accessibility of healthcare for a whole host of people. That includes those with mobility problems, those lacking access to care, and those in need of specialist services not readily available in remote locations.
Shortcomings of Telemedicine
We discussed earlier what the potential telemedicine benefits are. It’s only right that we also look at the potential pitfalls as well – because, as with all new technologies, there are a few downsides as well as all the upsides.
There are certain barriers that continue to hinder its expansion. These are both in terms of ingrained societal attitudes and habits with regard to healthcare, and also other barriers like age-related adoption. It’s important to recognise these so that, in time, they might be overcome.
But just what are the shortcomings of telemedicine, how do they affect take-up of remote, video-based medical services, and how far might they be surmounted in the years ahead? Let’s take a look.
The most obvious shortcoming, and one which continues to cause some concern for patients, is that the shift towards telemedicine may make in-person visits to doctors harder to come by. Again, this is partly an age-related factor – older people, generally not so used to using technology (especially for these purposes), maybe mistrustful and reluctant about making use of telemedicine services.
We’ve also discussed the budgetary constraints facing healthcare providers. There may be a temptation to scale back in-person medical services in favour of cheaper telemedicine consultations or video visits when a lot of patients either distrust the latter or would prefer to maintain a healthy balance of the two.

Of course, the fact is that telemedicine will never completely replace in-person visits to clinics, surgeries, and emergency departments. There will always be a need for physical examinations so that doctors can see for themselves what issues patients are suffering from. In addition, a lot of patients simply feel that telemedicine is somewhat impersonal – as if they’re being rolled along a conveyor belt before making way for the next patient. This is something of a misconception. The standard of the consultation will depend on the individual doctor concerned, although they are under their own constraints. It is a view that’s still quite widely held, though, and therefore important to bear in mind. It is a matter for healthcare providers to ensure that they do not make inappropriate efforts to cut back in-person treatments and consultations with telemedicine; each has its respective place.
Another potential issue with telemedicine is that it may, if not used with great care, lead to disruption in care continuity. This is a particularly important factor, especially for those patients with long-term health conditions or multiple problems.
Patients who use telemedicine services but don’t see the same doctor consistently may feel that the continuity of their treatment suffers as they’re being passed around from pillar to post. Telemedicine apps allow patients to sign in and request a consultation, but they may be given no real say in which doctor they speak with. This is a risk that telemedicine companies should be aware of, and they need to ensure that patients are connected with the same doctors consistently so that continuity doesn’t suffer.
For providers, too, there may be some initial drawbacks of introducing and scaling up telemedicine services. Most obviously, introducing telemedicine will come with certain costs involved. It goes without saying that the technology involved is far from cost-free, and then there are other overheads associated with that.
Doctors and other staff members will have to be trained in how to use and accommodate telemedicine services, perhaps forcing other changes to their working routine. All this has an effect on staff productivity, at least while people get up to speed with how the technology works and find ways of integrating it.

The guidelines and regulatory requirements of telemedicine may also be somewhat opaque for both patients and providers. Needless to say, healthcare bodies are well used to the necessities of patient confidentiality (it’s a key part of their professional code). Telemedicine, though, comes with its own specific demands and adjusting to these may prove something of a challenge in that initial introductory phase.
Patients should also be made aware of their rights and the protections afforded them when using telemedicine services. This will do a lot to reduce concerns about the technology, improve transparency, and encourage patients’ general take-up of telemedicine.
Terminology of Telemedicine
There is, as you’ve probably already noticed, rather a lot of terminologies to take in when you’re trying to get your head around telemedicine and how it works. Hopefully, we’ve done a good enough job up to now in holding your attention and explaining things in easy-to-understand language. We’ve tried so far to cover the different types of telemedicine services available, what they’re used for, and what the potential benefits of telemedicine to both patients and healthcare providers alike could be. Even though telemedicine has grown exponentially in recent years, a lot of patients are still unfamiliar with the ins and outs of it.

It may be helpful nonetheless at this point to break down the terminology of telemedicine, listing some of the most commonly used phrases and their meanings. Here’s a quick glossary
- Telemedicine: the provision of consultations, evaluations, diagnoses, and treatments from a healthcare provider to a patient via remote means perhaps using mobile devices. These include video (or audio) consultations, as well as remote monitoring and sharing of, for example, patient records or lab and test results.
- Telehealth: the use of telecommunications technologies to provide or support patient healthcare. Telemedicine would be considered a type or sub-category of telehealth, therefore.
- Informatics: the use of computer technologies for the purposes of processing and analysing data and information. The rise of big data means that informatics is becoming ever more important; it’s not just about collecting data but knowing how to analyse and make use of it.
- Diagnostic equipment: hardware devices distinct from a central computer which can be used to ascertain medical data and input it into a computer, or accept output from it. These devices might include, for instance, a stethoscope, digitisers, or a camera.
- Interactive video: video conferencing technology allowing for two-way, interactive, synchronous video exchanges. Telemedicine platforms incorporate this technology but do not operate in the same way as ordinary video conferencing apps, as they need much stricter security provisions to protect patient confidentiality.
- Telepharmacy: the provision of pharmacy services via remote means, such as audio or video link through telemedicine software. Provided when the in-person services of a pharmacist are unavailable or inaccessible.
- Teledermatology: remote treatments or consultation for patients’ skin problems.
- Telepsychiatry: the remote provision (including consultation, monitoring, and evaluation) of patients thought to be suffering from psychiatric health problems, thereby ensuring that those incapable of travel can receive care and evaluation.
- Teleradiology: the sharing of radiology test results (including x-rays and other imaging tests) between one location, for example, where the tests are conducted, and another, where the results are analysed and a diagnosis made. This would come under the category of store-and-forward, or asynchronous telemedicine.
- Telerehabilitation: the remote oversight and delivery of rehabilitation services to patients recovering from some sort of physical trauma or injury. As patients who have suffered a serious physical injury may struggle to travel, this is often a more convenient and practical solution.
- Application service provider (ASP): the company or healthcare body that provides telemedicine services. How these are accessed will depend on the nature of that healthcare provider. It may be paid for, depending on the location and the nature of the service, by a public health body, an insurer, or simply by an individual consumer buying a service directly from an ASP. Customers may, for instance, pay a regular subscription to telemedicine companies to access a specific service, such as on-demand video consultations.

Conclusion
So, we’ve now assessed the current state of telemedicine in the UK and worldwide. We’ve covered what it offers in terms of financial impact and healthcare outcomes, what it can do for patients and the range of services it currently incorporates. It’s worth now taking the time to consider also where it might go from here.
It’s already apparent that it’ll take quite some time for things to go ‘back to normal’ after Covid-19, and that’s assuming they ever do. What’s also clear is that the pandemic will have lasting impacts across a variety of different areas: these include how and where we work, how we communicate with each other, and how we access services.
Healthcare, it’s safe to assume, is one area that will be irrevocably changed by the virus. This means there will be opportunities and demand for telemedicine technology. Indeed, it is quite likely that telemedicine solutions will be used much more heavily in the future of healthcare to address the treatment of infectious diseases and reduce their spread.
We’ve already observed how doctors and healthcare providers are stepping up the rollout of telemedicine services to keep people out of surgery, clinic, and hospital waiting rooms. All the spaces where patients are at close quarters and viruses can easily spread. Telemedicine, as we’re seeing, can be used to provide patients with easy access to specialist help and advice without them having to venture out to healthcare facilities in person.
In the event of future or potential pandemics, we could see telemedicine rolled out quickly as a measure to restrain the spread of viruses.

Furthermore, it seems that telemedicine is set to be used – contrary to the fears of some – to strengthen relationships between patients and practitioners. That’s rather than reducing the former to mere consumers of the latter.
One of the crucial telemedicine benefits, as we’ve discussed at length here, is that it makes it far less of a rigmarole for patients to seek the input of a doctor when they feel ill or suspect something may be wrong. The thought of making an in-person trip to the doctor’s surgery can be quite a deterrent for some patients, but with telemedicine, it’s easy to check-in and discuss the problem from home. This should, it is hoped, encourage patients to seek more regular check-ups, ensuring that serious problems are diagnosed sooner and thereby potentially saving many lives.
Updated Jan 16, 2023



