The incredible, recent advancements in technology has sparked the adoption of telehealth – a new way for providing instant and timely medical care and consultation for patients at remote locations.
Telehealth is not merely using video conferencing tools, but it entails a gigantic transformation in technology, infrastructure, operational process, human resources, and doctor-patient relationship. Of all the change agents, technology is the factor that makes the biggest impact.
There are two technologies – online video conferencing and self-serving kiosks – both of which are changing the relationship between healthcare providers, patients, and medical facilities, for the better.
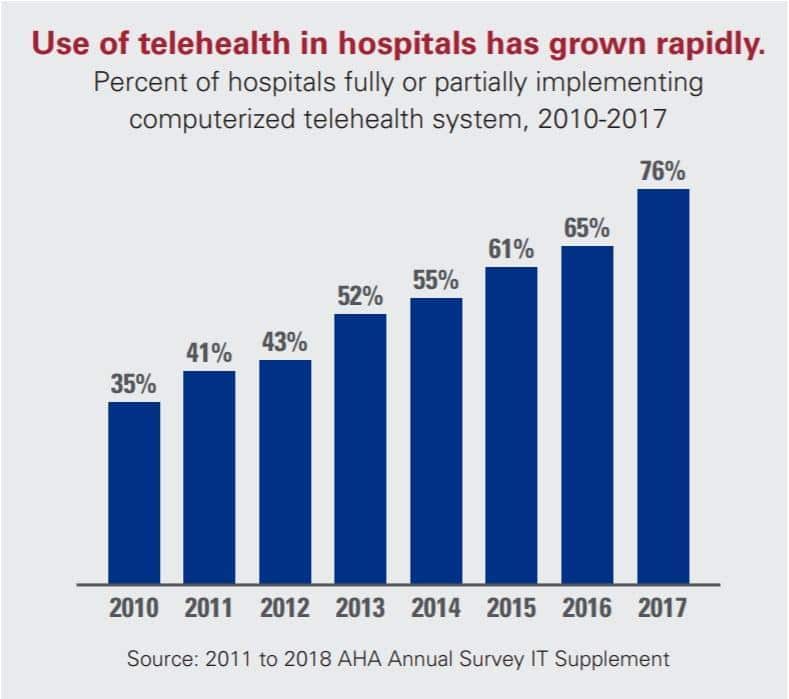
Image Source: telehealth factsheet from the American Hospital Association
Making medical appointments more accessible than ever for everyone
As we all know it could be a tedious process booking medical appointments and taking the time to travel back and forth just for one simple cheque-up. For people who live far away or are busy juggling multiple jobs, it’s very difficult to make the time for something that’s critically important.
One of the change agents that propel telehealth’s growth, as mentioned above, is technology. With the help of online video conferencing and self-serving kiosks at medical facilities, more and more people can now get medical support without sacrificing a chunk of their day.
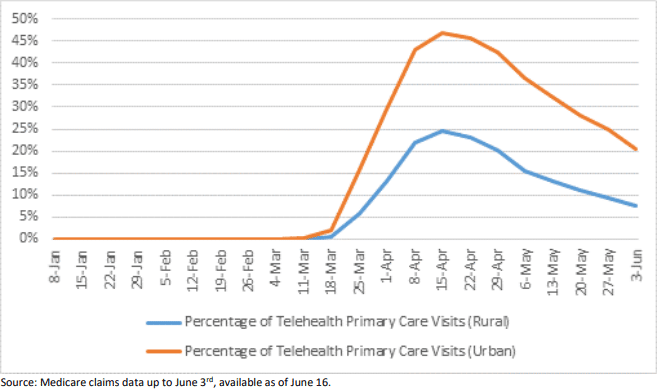
Image source: ASPE issue brief from the U.S. Department of Health & Human Services
At-home appointment using online video conferencing tools
With online video communication tools, doctors and patients can easily connect with real-time feedback. The ease of use of these tools also makes it easy to set up an appointment, which is especially convenient for people who live far away from the medical centre and often need to rely on public transportation for the long commute.
The time and cost alone for a simple appointment makes people reluctant to get help, which sometimes can be detrimental in missing the window to spot early symptoms of illness. For people who don’t have time to spare, like working multiple jobs or needing to take care of the family, an easy meeting online can also be a lifesaver. Patients can easily cheque in with doctors to determine if an in-person examination is needed.
Using self-serving kiosks to save time from administrative procedures
As self-serving kiosks have been seeing wider adoption throughout many industries, notably retail, servicing, and public spaces, the trend is also making an impact for the healthcare industry. Hospitals and medical facilities can set up kiosks for patient cheque-in, building directory & wayfinding, patient information logging, payment, and much more.
Imagine this: before a patient walks into an appointment, he or she can cheque-in using a kiosk without needing a staff writing down all the information by hand and manually typing it into the computer. If a patient needs to go through a series of examinations, the directives can be provided by a kiosk. If there’s going to be another appointment, the patient can use the kiosk to see the details and print out the information for record-keeping.
Having self-serving kiosks can save patients and medical staff a lot of time from waiting just for administrative procedures to be done. The kiosks can also be placed throughout the facility, so patients have easy access.
Improve the quality of care for chronic diseases
For patients who have a chronic illness and need to regularly go to a medical facility for cheque-ups, telehealth can save them from having to commute back and forth. Although it’s not only just saving time for patients, it’s better resource allocation for every party involved. The benefits include:
- Rural residents can also get the same degree of medical support: with around 57 million Americans currently living in a rural area, many patients often have difficulty accessing medical facilities. Not only do they need to travel long distances for each appointment, but the cost is also another big concern. The biggest benefit is that patients can still get support from the comfort of their homes.
- Doctors can monitor patient lifecycle changes: with telehealth technologies, doctors can cheque in with patients on a regular basis and make lifestyle adjustments including diet selection, sleeping patterns, or exercising frequency. With timely feedback and assessment, patients can get concrete advice in building a sustainable recovery plan.
- New symptoms can be spotted early: patients with chronic illness sometimes can see minor new symptoms that may or may not have anything to do with the illness. When a patient can’t regularly cheque back in with the care provider due to time, travel distance, or cost concern, the new symptoms are often overlooked. However, with telehealth technologies like online video calls, doctors can spot abnormal symptoms and act fast to prevent the illness from getting worse.
- Reduce hospital readmissions: patients with chronic diseases make up most admissions. When care providers can remotely monitor and manage patient lifestyle, it can help reduce the chances of being readmitted. This also reduces the cost of care for both patients and care providers.
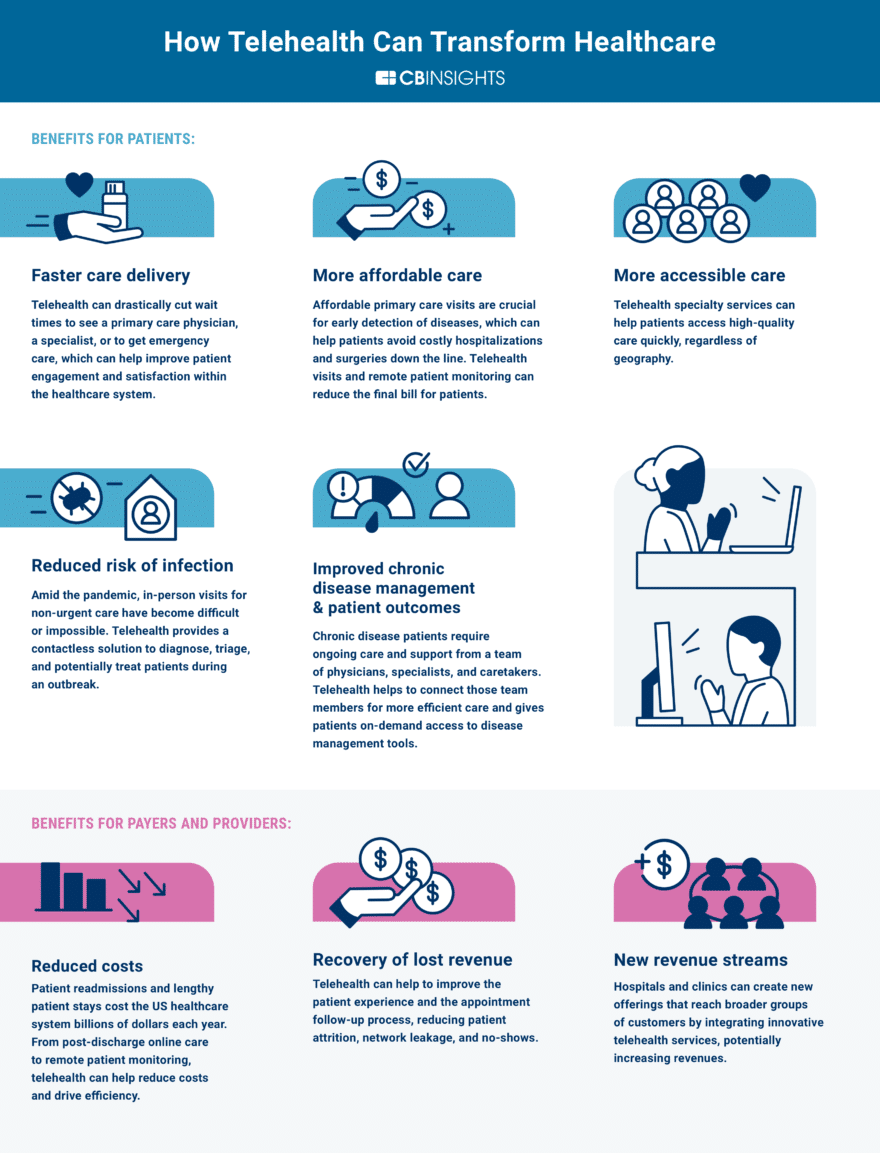
Image Source: https://www.cbinsights.com/research/telehealth-transform-healthcare-post-covid-19/
Doctor-patient relationship and experience can be improved
The ability for doctors to provide medical advice and get real-time feedback from the patients all without having to leave home can greatly improve the relationship and the quality altogether.
- It’s more relaxing when both parties are at home: the home environment makes it a lot more relaxing for each appointment session. For care providers, they won’t feel like they are at the hospital and everything is being watched. It feels like more of a casual chat and takes the pressure off the care providers but can still get the job done. For patients, the comfort of being home can help take the edge off and thus might be more willing to share information about their health conditions.
- Regular appointments can help doctors learn more about the patients: when it’s not easy to establish regular cheque-ins with your patients due to time conflict and inconvenience for the patients to come back to the hospital, the care providers can only rely on medical and appointment records.
Now since it’s easier for both parties to connect with each other with more flexibility in terms of schedule and frequency, doctors can get to know the patients better on a personal level. When a healthy and positive relationship is established, the overall quality and experience can be greatly improved since more details, real-time feedback and communication can be provided.
Making admin processes at medical facilities much more efficient
Another big technology that can help reduce workload and increase efficiency for the entire process and experience is self-serving kiosks. When patients do need to go to the hospital, much of the time is often spent filling out forms, waiting in line, finding directions, and many more administrative processes. Here are some common use cases:
- Patient check-in kiosk: when patients can cheque-in without any assistance, your staff can focus on higher-level tasks that ultimately help with improving patient experience. During the cheque-in, the software can verify patient information and if needed, ask patients to fill in missing data to complete the profile. Hospitals can have the latest patient information without manually checking with the patients. All the kiosks are connected to streamline the process.
- Building directory & wayfinding: patients, visitors, and vendors can leverage the wayfinding kiosk to function as a virtual front desk and show directions for the visitors to easily find where they need to go.
- HR kiosk for care providers & staff: internal staff can also use kiosks to clock in and out, print documents, manage PTO, make various administrative requests.
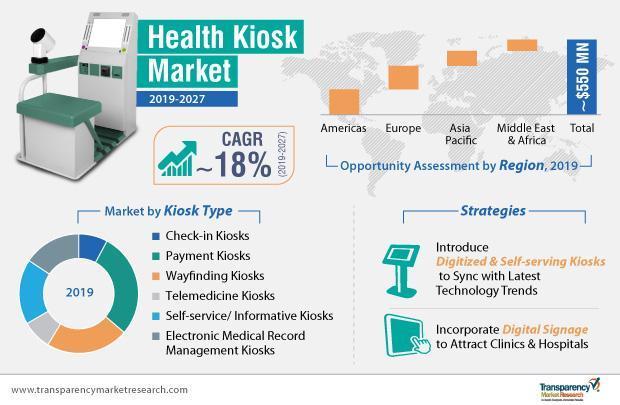
Image Source: transparency market research on health kiosk market
In addition to bringing in physical kiosks with specialised software built to streamline various processes, there is also software like device lockdown solutions that ensure the kiosks can work the way they are intended for. Device lockdown solutions can allow IT managers to lock the kiosk down to just the one application (cheque-in portal, wayfinding, and any other specialised application) and visitors aren’t able to tamper with the kiosk.
Lower cost and better allocation of resources for everyone
One of the benefits of implementing telehealth services like online video conferencing and self-serving kiosks is to help lower overhead costs and better allocate resources:
- Reduction in patient transportation and inter-hospital transfers: through remote cheque-in using online video conferencing tools, doctors can keep watch on patients’ health status and conduct regular appointments without asking patients to spend hours travelling to a physical office.
- Fewer readmissions to ER: by screening and learning the patient’s health status using a quick online appointment, situations that don’t require ER treatment can be redirected to other resources or medical support. This will greatly improve the ER workload, both for the equipment, financial and human resources that need to be invested on a daily basis. Now ER can be used for critical emergencies.
- Kiosks help cut down waiting and manual administrative work: by setting up self-serving kiosks to help with patient cheque-in and collect necessary information, there’s no need to assign staff to manually organise the data and log them into a computer. More staff can focus on higher-level tasks to improve the quality of the services they provide to patients. When everything is centralised and synced to one place, everyone will have access to the latest information they need.
- Transform physical offices to more hospital beds: as more care providers can conduct medical appointments online, hospitals can reduce the number of physical offices and create more hospital beds for more patients that do need specialised medical care.
How to create a solid foundation of your telehealth service?
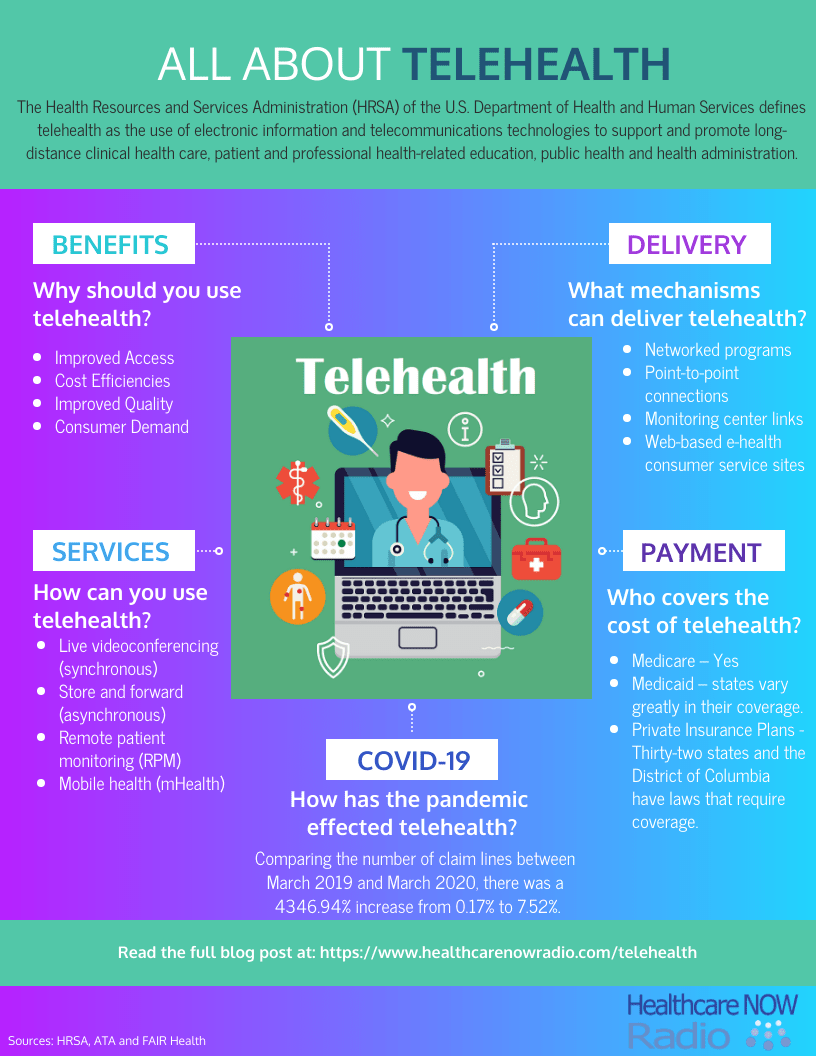
Image Source: https://www.healthcarenowradio.com/all-about-telehealth/
Implementing telehealth-related technologies is just one of the things that you should do to drive the transformation. To build a sustainable and scalable telehealth service for your patients, you need to consider factors like:
- The scope of your services: it could range from just providing online video conferencing, or it could expand to have omnichannel communication capabilities for patients to easily get access to medical support & advice even if they are at home.
- The features you need: do you just need 1-to-1 communication or do you need a team of care providers to join in on a call and collaborate on a case?
- Training for your staff (and for the patients): when you are making the transition to incorporate telehealth services, you need to provide education for the care providers, including using the telehealth technologies to be more effective and efficient, staying in touch with patients, and be well-versed in navigating the software and tools.
Your care providers might also need to provide guidance and directions when connecting with the patients as most people aren’t used to using technology tools for medical appointments. Your IT team should also have the ability to provide support remotely when the software or devices used for telehealth aren’t working properly as they should.
- Security: maintaining the security of data transmission, data storage, information sharing, and patient privacy is critical for medical facilities when implementing telehealth services. It’s also necessary that the care providers and tech support are well trained with hospital regulations and are able to communicate and explain the process to the patients.
- Cost control: telehealth can help hospitals and medical facilities save on overhead costs, but coordinators and IT managers that help plan and set up the infrastructure and tools need to make sure that they choose the right solutions that fit their needs. The rollout can be divided into stages so things can be tested out to see if there are any adjustments that need to be made.
The last thing you want to do is spend millions of dollars implementing infrastructure and solutions that don’t work well with your facilities, medical staff, and IT support team. With the right solutions in place, telehealth services can not only help save unnecessary costs but also free up more resources for everyone.
Care providers who are looking to implement telehealth services can visit telehealth.hhs.gov to find tips for building workflows and getting started.
Updated Jan 16, 2023